Browse our range of reports and publications including performance and financial statement audit reports, assurance review reports, information reports and annual reports.
Efficiency of Veterans Service Delivery by the Department of Veterans’ Affairs

Please direct enquiries through our contact page.
The objective of this audit was to assess whether the Department of Veterans’ Affairs is efficiently delivering services to veterans and their dependents.
Summary and recommendations
Background
1. The Department of Veterans’ Affairs (DVA) provides support to current and former Australian Defence Force (ADF) members and their families, ranging from financial support, treatment and services. DVA administers financial and services support under three main pieces of legislation: the Veterans’ Entitlement Act 1986 (VEA); the Military, Rehabilitation and Compensation Act 2004 (MRCA) and the Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 (DRCA).
2. DVA supported approximately 165,000 veterans and more than 125,000 dependents in 2016-17 at a cost of more than $12 billion.
3. DVA has approximately 2,000 staff with offices in every State and Territory. Its work is delivered through specialised service delivery programs distributed across its offices.
Rationale for undertaking the audit
4. In August 2017, the Senate Standing Committee on Foreign Affairs, Defence and Trade delivered its report following an inquiry into suicide by veterans and ex-service personnel; The Constant Battle: Suicide by Veterans. The report stated that: ‘The need to streamline the administrative practices of DVA was the overwhelming concern of the majority of submissions to the inquiry’. Report Recommendation 13 was that the Australian National Audit Office commence the proposed performance audit of the efficiency of veterans’ service delivery by DVA as soon as possible.
5. Additional factors supporting the conduct of the audit included:
- Commencing in 2017–18, the Government provided DVA with $166.6 million over four years to begin transforming and improving services to more effectively and efficiently meet the current and future needs of veterans and their dependents. The measure is titled ‘Veteran Centric Reform’. The audit examined some of the results of DVA’s early implementation of the reform.
- A Functional and Efficiency Review (May 2016) of DVA recommended that service delivery functions either be outsourced or transferred to other agencies. The review stated that the reform would lead to ‘administrative efficiencies’. This audit included analysis of the efficiency of DVA’s Rehabilitation and Compensation (R&C) processes.
Audit objective and criteria
6. The objective of the audit was to assess whether DVA was efficiently delivering services to veterans and their dependents. To form a conclusion against the audit objective, the Australian National Audit Office (ANAO) adopted the following high-level audit criteria:
- Do business systems and processes in DVA support the efficient delivery of services to veterans and their dependants?
- Have compensation, support and health services been delivered efficiently by DVA to veterans and their dependants?
Conclusion
7. The majority of DVA Rehabilitation & Compensation (R&C) services are being delivered to veterans and their dependents within DVA’s time based performance targets, however a minority of claims take an excessively long period to process due to inefficient handling. These delays can have significant impacts for these veterans.
8. The audit identified weaknesses in DVA’s business systems and processes, which do not adequately support the efficient delivery of services. In particular, DVA should improve the structure and consistency of workflow management for R&C claims, and review its highly segmented approach to processing claims under the various elements of applicable legislation. DVA’s focus on monitoring the median and the average time taken to process (TTTP) across the population of claims does not provide a sufficiently complete picture of performance, and does not address critical reputational and client welfare risks.
9. For claims with a high TTTP, the audit identified that this stemmed from excessive time associated with ‘inactivity’ (delays in the actioning of a claim despite the presence of required information) and medical reviews. DVA should improve its oversight of the progress of individual claims through the processing lifecycle, and its management of medical service provision. The monitoring and reporting of claims is not effective in alerting management to those which are at risk of taking excessive time to process.
Supporting findings
Business systems and processes
10. Whilst a high level workflow methodology has been established for R&C claims, the Rehabilitation and Compensation Integrated Support Hub (ISH) system is not being used to support compliance and management of workflow, but rather as a repository of records associated with a claim at the completion of processes.
11. ISH workflow management has been replaced in practice by individual spreadsheets maintained in various formats.
12. DVA’s approach to claims allocation and management means that claims can be ‘lost’ in the various hand-off points between areas, causing delays and inefficiencies.
13. R&C processes for VEA claims are designed as an end-to-end process. However, R&C processes for DRCA and MRCA claims are not designed to maximise efficiency. The approach to assessment for these claims is resulting in the unnecessary disaggregation and re-aggregation of components within some DRCA claims, information requests to third parties being lodged multiple times for the same claims and multiple areas of DVA being required to review the same voluminous case files.
14. In the ANAO sample, information requests from the Department of Defence and medical specialists took a large proportion of the elapsed TTTP for a claim. DVA’s internal targets and external reporting for R&C claims are not well aligned to the current agreement with the Department of Defence.
15. DVA reporting indicates that the average TTTP fell between 3 per cent and 9 per cent across all R&C claim categories in the period 2015 to 2017. Reporting also indicates that the number of cases-on-hand / work-in progress has fallen by 17.9 per cent (2,266) across the same period, and the average age of cases by between 16 per cent and 45 per cent across the relevant claim categories.
16. DVA’s focus on the use of the median and the mean TTTP in both operational and external reporting for the performance of the R&C business does not provide a sufficiently complete picture of performance. In addition, it does not necessarily address critical risks given that even a small number of very high TTTP claims can have significant impacts for veterans and DVA’s reputation.
17. Testing identified inconsistencies in naming conventions for records in ISH and HP Content Manager, DVA’s primary records management system. Locating all relevant documentation associated with a claim during the testing process was inefficient and time consuming.
18. It is apparent that the ISH system does not have controls to ensure integrity over the high volume of manual records placed in the system. This was particularly evident in relation to the dates associated with registration of claims and referral for medical consultations. Instances were also identified where key client documentation was being kept manually by staff for periods prior to lodgement in the ISH system.
Delivery of services
19. Testing indicated that the two main drivers of high TTTP claims were the need to wait for responses from medical specialists, and ‘inactivity’.
20. Unlike the Single Access Mechanism (SAM) arrangements with the Department of Defence, there is no formal control or monitoring of requests for information from medical specialists. Time spent waiting for responses from medical specialists in the ANAO’s testing was, on average, 10 times greater than for information requests to the Department of Defence.
21. There were two main reasons for ‘inactivity’: where claims were effectively ‘lost’ in the system; and where the delegate did not immediately take action after requested information was received and the claim was actionable. Both issues are indicative of a lack of transparency over workflow within the system.
22. DVA has an internal Quality Assurance function which conducts a statistically based review of all DVA activities. The error rate was above tolerable levels for 2016-17 in three of the six primary R&C claim categories.
23. An extensive suite of reports and analysis is prepared at various frequencies containing key metrics and analysis on R&C operations. This reporting has limited analysis about emerging risks or the reasons behind changes in performance. Management reporting does not identify progress on claims or the reasons for any delays, and is largely unutilised by team leaders.
24. The significant reorganisation of R&C operations following the creation of a national R&C business in 2015 has meant that internal benchmarking by location does not currently provide reliable comparisons. Comparisons between processing locations will become more reliable, as measures relative efficiency, when more comparable data becomes available.
25. Comparisons between DVA and Comcare show significant differences in approach to claims processing. However, there may be value to DVA in implementing comparisons based on trends or detailed processes.
Recommendations
Recommendation no.1
Paragraph 2.20
The ANAO recommends that DVA establish appropriate workflow management over R&C processes that will allow for identification of potentially problematic claims and delays in processing earlier in the claims investigation process.
Department of Veterans’ Affairs response: Agreed.
Recommendation no.2
Paragraph 2.44
The ANAO recommends that DVA review the current approach to processing R&C claims to address efficiency issues including aggregation and disaggregation of DRCA claims, multiple instances of information requests to third parties and the number of staff involved in the processing of individual claims.
Department of Veterans’ Affairs response: Agreed.
Recommendation no.3
Paragraph 2.65
The ANAO recommends that DVA implement claims processing targets that include consideration of the distribution of the TTTP as well as the average/median.
Department of Veterans’ Affairs response: Agreed.
Recommendation no.4
Paragraph 2.78
The ANAO recommends that DVA addresses weaknesses in information and records management, in particular: retention of records outside of primary systems, inconsistent use of naming conventions, and ensuring the completeness and accuracy of client records.
Department of Veterans’ Affairs response: Agreed.
Recommendation no.5
Paragraph 3.21
The ANAO recommends that DVA implement greater control and monitoring over its requirement for information from medical specialists. This should include contractual arrangements that prescribe timeliness and quality for independent medical specialists engaged directly by the DVA and prompt and frequent follow up where the client has elected to use their own treating medical specialist.
Department of Veterans’ Affairs response: Agreed.
Recommendation no.6
Paragraph 3.40
The ANAO recommends that DVA develop and implement R&C reporting into its RACER system that:
- will allow the identification of claims that are potentially problematic at an individual claim level for operational management and at an aggregated level for oversight and governance; and
- provides transparent flow of consistent information at levels suitable for governance, module management and team and individual performance management.
Department of Veterans’ Affairs response: Agreed.
Summary of entity response
26. The Department of Veterans’ Affairs notes the results of the audit and thanks the Australian National Audit Office for the opportunity to respond to the issues raised. The Department notes and agrees with the six recommendations outlined in the audit report.
Key learnings for all Australian Government entities
Below is a summary of key learnings, including instances of good practice, which have been identified in this audit that may be relevant for the operations of other Commonwealth entities.
Governance and risk management
Contract management
Records management
1. Background
Introduction
1.1 The Department of Veterans’ Affairs (DVA) provides support to current and former Australian Defence Force (ADF) members and their families, ranging from financial support, treatment and services. Support is available for such individuals where injury, disease, death, permanent impairment, incapacity for work or service or loss or damage to medical aids has occurred and where ongoing household, attendant or health care is required. DVA administers financial and services support under three main pieces of legislation: the Veterans’ Entitlements Act 1986 (VEA); the Military, Rehabilitation and Compensation Act 2004 (MRCA) and the Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 (DRCA).
1.2 DVA supported approximately 165,000 veterans and more than 125,000 dependents costing more than $12 billion in 2016-17.
1.3 As at 30 November 2017 DVA had a total of 1,967 employees. DVA has offices in all States and Territories of Australia, with the aim of providing nationwide support and assistance to all current and former ADF members.
1.4 DVA is responsible for three outcomes as illustrated in Table 1.1.
Table 1.1: DVA Outcome structure
|
|
OUTCOME 1: Compensation and Support |
||||
| DEPARTMENT OF VETERANS’ AFFAIRS
|
Maintain and enhance the financial wellbeing and self-sufficiency of eligible persons and their dependants through access to income support, compensation, and other support services, including advice and information about entitlements. |
||||
|
PROGRAMS |
1.1: Veterans’ Income Support and Allowances |
1.2: Veterans’ Disability Support |
1.3: Assistance to Defence Widow(er)s and Dependants |
1.4: Assistance and Other Compensation for Veterans and Dependants |
|
|
1.5: Veterans’ Children Education Scheme |
1.6: Military Rehabilitation and Compensation Acts Payments - Income Support and Compensation |
1.7: Adjustment to the Military Rehabilitation and Compensation Acts Liability Provision - Income Support and Compensation |
|
||
|
OUTCOME 2: Health |
|||||
|
Maintain and enhance the physical wellbeing and quality of life of eligible persons and their dependants through health and other care services that promote early intervention, prevention and treatment, including advice and information about health service entitlements. |
|||||
|
PROGRAMS |
2.1: General Medical Consultations and Services |
2.2: Veterans’ Hospital Services |
2.3: Veterans’ Pharmaceuticals Benefits |
2.4: Veterans’ Community Care and Support |
|
|
2.5: Veterans’ Counselling and Other Health Services |
2.6: Military Rehabilitation and Compensation Acts - Health and Other Care Services |
2.7: Adjustment to the Military Rehabilitation and Compensation Acts Liability Provision - Health and Other Care Services |
|
||
|
OUTCOME 3: Commemorationsa |
|||||
|
Acknowledgement and commemoration of those who serve Australia and its allies in wars, conflicts, and peace operations through promoting recognition of service and sacrifice, preservation of Australia’s wartime heritage, and official commemorations. |
|||||
|
PROGRAMS |
3.1: War Graves and Commemorations |
3.2: Gallipoli-related Activities |
|||
Note a: Outcome 3 is not within the scope of this audit.
Source: DVA Annual Report 2016–17.
Legislative functions
1.5 The VEA applies to military service between 7 December 1972 and 30 June 2004. The Act provides for pensions and allowances encompassing disability pension, special rate pension, temporary special rate pension, intermediate rate pension, extreme disablement adjustment, war widow(er) pension, orphan’s pension and additional provisions for specific disabilities and allowances.
1.6 The DRCA provides compensation for injuries, diseases or deaths resulting from service between 3 January 1949 and 30 June 2004. The benefits available to veterans include medical and treatment expenses through a DVA Health Card, incapacity payments, permanent impairment lump sum, rehabilitation and help to return to work, and household and attendant care services.
1.7 The MRCA provides rehabilitation and compensation support for current and former members of the ADF with service on or after 1 July 2004. The MRCA provides for support including permanent impairment compensation, incapacity payments, special rate disability pension and compensation following death.
1.8 The timing of a veteran’s service and the timing of the causal event may result in the application of multiple Acts to a single claim and this affects the way the claim is processed. For example:
- each of the Acts has specific requirements about how claims should be treated;
- the VEA and the MRCA require consideration of claims holistically, whereas the DRCA requires consideration of individual conditions; and
- the VEA and the MRCA require the beneficial treatment of veterans’ claims.1
- In addition, DVA has adopted a policy position of actively assisting veterans in submitting claims under the legislation.
Transaction volumes and client demographics
1.9 DVA’s total expenditure for the 2016-17 financial year was $12.1 billion. A breakdown of this expenditure for Outcome 1 and Outcome 2 by legislation is shown in the table below.
Table 1.2: Total 2016-17 financial year spend for each outcome under legislation
|
|
VEA |
MRCA |
DRCA |
|
Outcome 1 |
$5,480 million |
$383.5 million |
$142.6 million |
|
Outcome 2 |
$4,510 million |
$84.6 million |
$41.7 million |
Source: DVA Annual Report 2016-17.
1.10 In 2016-17 DVA provided services to 176,232 income support clients, 169,727 compensation clients and 94,726 Veterans and Veterans Families Counselling Service clients. At June 2017, clients held 135,263 Gold Health Cards and 58,705 White Health Cards issued by DVA.
1.11 A Gold Card entitles the holder to DVA funding for services for all clinically necessary health care needs, and all health conditions, whether they are related to war service or not. The card holder may be a veteran or the widow(er) or dependant of a veteran.
1.12 A White Card entitles the holder to care and treatment for:
- accepted injuries or conditions that are war caused or service related;
- malignant cancer, pulmonary tuberculosis, any mental health condition whether war caused or not; and
- the symptoms of unidentifiable conditions that arise within 15 years of service (other than peacetime service).
1.13 Services covered by a DVA White Card are the same as those for a Gold Card but must be for one of the above conditions.
1.14 As at September 2017 DVA had a total of 288,358 clients. This comprised 218,397 VEA clients, 26,455 MRCA clients and 52,163 DRCA clients. The larger number of VEA clients reflects the length of time that the VEA and its predecessor Acts have been in force. In 1986 the VEA repealed five Acts that made provision for entitlements for repatriated veterans, consolidating legislation that had been in effect since 1920 and covered many of the major conflicts of the twentieth century. The superseded legislation included:
- Repatriation Act 1920;
- Seaman’s War Pensions & Allowances Act 1940;
- Repatriation Far East Strategic Reserve Act 1957;
- Repatriation (Special Overseas Service) Act 1962; and
- Repatriation (Torres Strait Islanders) Act 1972.
1.15 The pattern of coverage is also reflected in the age profile of DVA’s clients. This is illustrated in Table 1.3.
Table 1.3: DVA client age profile
|
|
Legislation |
||
|
Age Category |
MRCA |
DRCA |
VEA |
|
Under 30 |
23.8% |
0.1% |
1.3% |
|
30–34 |
20.1% |
2.4% |
0.3% |
|
35–39 |
15.6% |
8.0% |
0.5% |
|
40–44 |
12.0% |
12.9% |
0.9% |
|
45–49 |
11.2% |
17.6% |
2.5% |
|
50–54 |
7.7% |
14.7% |
3.5% |
|
55–59 |
5.3% |
13.1% |
4.6% |
|
60–64 |
3.2% |
9.8% |
7.0% |
|
65 - 69 |
1.0% |
9.2% |
15.6% |
|
70–74 |
0.2% |
6.2% |
15.4% |
|
75–79 |
0.0% |
2.9% |
7.5% |
|
80–84 |
0.0% |
2.1% |
7.2% |
|
85 or over |
0.0% |
0.9% |
33.7% |
Source: DVA Stats at a Glance, September 2017.
1.16 Table 1.4 sets out the range of services provided by DVA.
Table 1.4: DVA services
|
DVA services |
Details |
|
Health Care |
DVA provides a broad range of health care and support services to meet the clinical needs of eligible veterans and eligible dependents. DVA provides Gold Health Cards (all Conditions within Australia) and White Health Cards (accepted conditions). DVA also provides for Non–liability Health Care where immediate access to services is considered necessary. |
|
Transport |
The Repatriation Transport Scheme (RTS) allows DVA to provide a pre-booked taxi or hire car service, under the Booked Car Scheme (BCS) for travel to approved treatment locations for certain health card holders. |
|
Rehabilitation |
Rehabilitation is designed to assist former ADF members, cadets and declared members who have sustained an injury or contracted a disease due to their ADF service and have eligibility under the DRCA and/or the MRCA. |
|
Mental Health |
The Veterans and Veterans Families Counselling Service (VVCS) provides free and confidential, nation-wide counselling and support to eligible serving and ex-serving members, and their families affected by war and service-related mental health and well-being conditions. |
|
Incapacity Benefits |
Incapacity benefits are payments for economic loss due to the inability (or reduced ability) to work because of injury or disease that has been accepted as service related. Incapacity benefits can be made to current and former ADF members. |
|
Permanent Impairment payment |
Current and former ADF members who have an injury or disease as a result of their ADF service, and that injury or disease has left them with some permanent impairment, may be entitled to receive compensation for that impairment from DVA. This compensation is called permanent impairment (PI) payment. |
|
Pensions - Income Support |
Service pension provides a regular income for people with limited means. A service pension can be paid to veterans on the grounds of age or invalidity, and to eligible partners, widows and widowers. It is subject to an income and assets test. |
|
Pensions - Disability Compensation |
Disability pension is paid under the VEA to compensate veterans for injuries or diseases caused or aggravated by war service or certain defence service rendered on behalf of Australia before 1 July 2004. The amount of disability pension paid depends on the level of incapacity suffered as a result of war-caused or defence-caused injuries and diseases. |
|
Pensions - War widows and widowers |
War widow/er’s pension is paid under the VEA to compensate widowed partners of veterans who have died as a result of war service or eligible defence service. Orphan’s pension may also be payable to dependent children of deceased veterans. |
|
Compensation following death |
Compensation may be provided under the MRCA to the dependents of deceased members and former members of the ADF who die or were severely injured as a result of their service on or after 1 July 2004. |
|
Housing and Loans Assistance |
DVA administers the Defence Home Ownership Assistance Scheme (DHOAS) on behalf of the Department of Defence. DHOAS is available to current and former ADF personnel, and their surviving partners, who have served in the ADF after 1 July 2008, completed a qualifying period and accrued a Service Credit. |
|
Defence Service Homes Insurance Scheme |
Defence Service Homes Insurance Scheme (DSHIS) provides economical home, contents and other personal insurance to all persons who are eligible under the Veterans’ Entitlement Act 1986. |
Source: DVA website.
Changing operational demands and demographics of DVA’s client base
1.17 In its 2013 Capability Review: Department of Veterans’ Affairs (Capability Review), the Australian Public Service Commission (APSC) stated that ‘the environment in which DVA operates has changed at a much faster pace than the speed with which the department has allowed itself to change’.
1.18 One driver of change facing DVA is the changing age of its client base. The patterns of major war and warlike incidents in history has meant variability over time in the number of clients seeking DVA’s services, along with an overall reduction in the number of clients seeking those services. The changing age of DVA’s client base is illustrated in Figure 1.1.
Figure 1.1: Changing client population 2002-2017
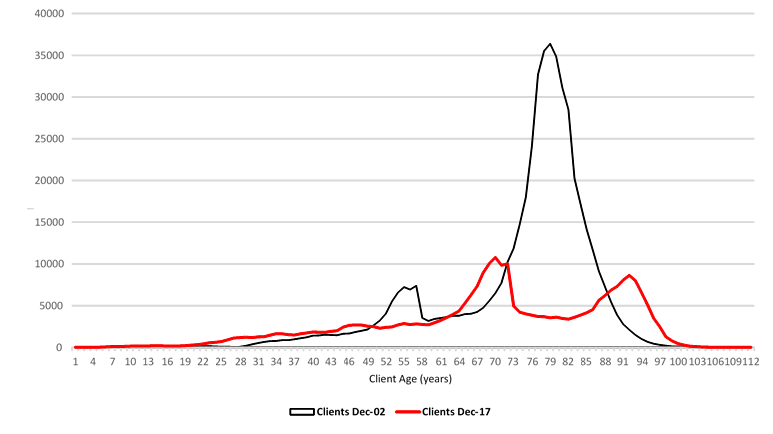
Source: DVA Client Statistics.
1.19 The potential impact of changes in the age profile of DVA’s client base is illustrated in Figure 1.2, which shows a difference in the levels of satisfaction with DVA’s services between older veterans and younger veterans. Survey results indicate that younger veterans (under 45 years of age) are less satisfied with every aspect of DVA’s service delivery. The areas of greatest difference between older and younger veterans in the survey results are: confidence in DVA and timeliness of DVA services.
Figure 1.2: Client satisfaction demographics
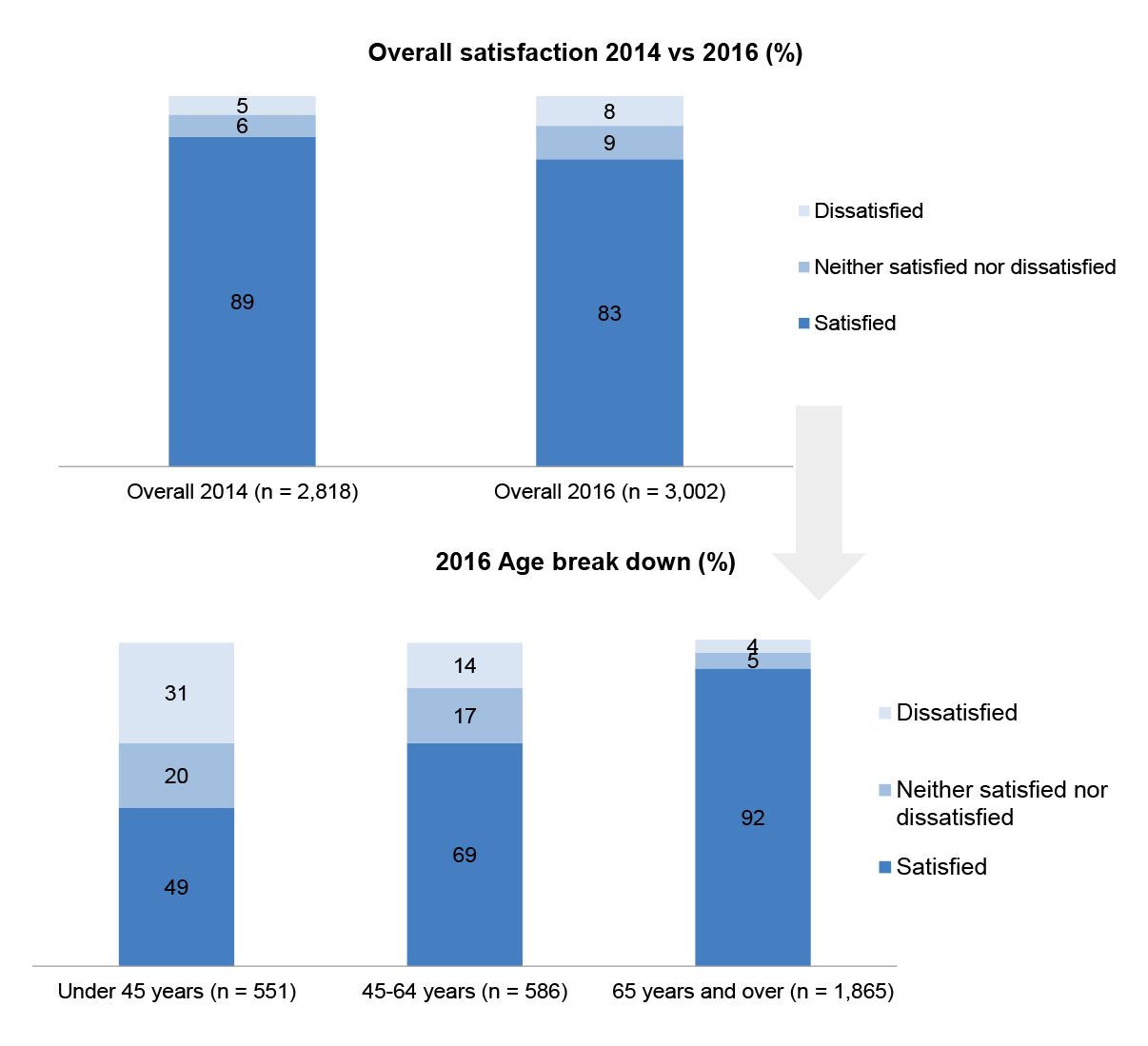
Source: DVA 2016 Client Satisfaction Survey.
1.20 One key area of difference between older and younger veterans identified in the survey was the preferred method of interacting with DVA. Fifty-five per cent of veterans under 45 years of age were willing to interact with DVA digitally, compared to 27 per cent of veterans over 45 years of age. In its 2013 Capability Review, the APSC summarised the challenge to DVA as ‘the older client base continues to decline while the new younger client base has different expectations.’
Internal change and transformation
1.21 Along with challenges represented by changing client demographics, a frequently identified challenge is that DVA service delivery relies on the use of more than 200 ageing information technology software systems. In a supporting paper for the 2017-18 budget for Veteran Centric Reform, DVA concluded that ‘DVA operations and infrastructure are no longer fit for purpose as current business systems are claims based, requiring the veteran to approach the Department, and lack the information sharing and data analysis necessary to meet veterans’ expectations of a quality service’.2
1.22 The APSC Capability Review also recognised these challenges and identified three areas ‘needing urgent attention for DVA to transform:
1. operating structure, governance arrangements and information and communications technology (ICT)
2. approach to clients, culture and staffing
3. efforts to formulate effective strategy, establish priorities and use feedback.’
1.23 To address the external and internal challenges it faces, DVA has embarked on the Veteran Centric Reform (VCR). The VCR is a six year transformational program that commenced on 1 July 2017. The government has provided first year funding of $166.6 million to assist DVA in this program. The reform aims to transform business processes and culture, improve service options and information and communication technology redevelopment. The reform’s initiatives are intended to support DVA’s clients and their families and focus particularly on enabling younger veterans to gain early access to treatment and support and improve the transition from the ADF to civilian life.
1.24 In addition to the VCR funding, in the 2017-18 Budget the Government provided $13.5 million to assist in claims processing, alleviate pressure on DVA staff and reduce the backlog of claims. The Government also provided $4.0 million over two years to pilot a veteran centric case management service for ‘at-risk’ veterans.
1.25 The VCR program is being delivered through nine work streams, which include four enabling work streams and five delivery work streams. Enabling work streams support access to data, change management and operational process improvements while the service delivery work streams deliver changes to veteran facing services.
1.26 One initiative of the VCR is to redesign the means of client interaction with DVA through the Digital Client Experience Stream. This stream has implemented the MyService platform to allow clients to complete applications online.
1.27 In February 2018 a Department of Finance Gateway Review3 was undertaken. This review concluded that progress in implementation of the VCR was ‘amber/green’4 and did not identify significant risks to the transformation project.
1.28 Whilst the VCR represents a significant transformation of DVA business operations, it is not the first or only change program underway in DVA. In 2013 the Department of Finance reviewed DVA’s information technology systems and concluded that the systems supporting Rehabilitation and Compensation (R&C) processes had ‘a high risk of catastrophic failure’. Subsequent to this, DVA applied for, and received budget funding in the 2016-17 Budget, of $23.9 million over two years to implement the Improving Processing Systems (IPS) Project.
1.29 In November 2014, the DVA Secretary announced a new R&C operating model to drive further improvements. This involved changing to a capability based structure and introducing Senior Responsible Officers for key functions. The new approach involved a move to a national business model rather than state based operations.
1.30 DVA has also announced changes aimed at improving the timeliness and quality of service delivery to veterans in the interim including:
- extending early access to treatment through Non-Liability Health Care for all mental health conditions for any veteran with one day of service or more;
- the implementation in 2017 of interim payments for Permanent Impairment (PI) cases;
- extending the use of Statements of Principle5 (SOPs), Streamlined Processing and Straight-Through Processing6 to simplify and speed up the determination of less complex claims.
Audit approach
1.31 The objective of the audit was to assess whether DVA was efficiently delivering services to veterans and their dependents. To form a conclusion against the audit objective, the Australian National Audit Office (ANAO) adopted the following high-level audit criteria:
- Do business systems and processes in DVA support the efficient delivery of services to veterans and their dependants?
- Have compensation, support and health services been delivered efficiently by DVA to veterans and their dependants?
1.32 The audit focusses on examining efficiency in terms of the relationship between inputs, outputs and the resources used by DVA to deliver services to its clients. The scope of the audit did not include:
- any services that DVA was not directly responsible for delivering and that were delivered jointly with another Australian Government entity, for example, Department of Human Services; and
- services delivered under DVA’s Outcome 3: Commemorations, which does not focus on payments and support services.
1.33 In order to minimise any duplication of the work of the Productivity Commission related to its current inquiry (27 March 2018) into Compensation and Rehabilitation for Veterans, the ANAO liaised with representatives of the Commission to discuss the scope and approach for the audit.
1.34 The audit comprised two phases, the first involved a broad examination of DVA’s activities across Outcome 1 and Outcome 2 to identify areas where a deeper examination of efficiency would be most valuable. The second phase involved a detailed analysis and transaction testing of those areas identified in phase one. The review spanned transactions under the three relevant Acts, and was targeted primarily on the R&C activities of DVA. DVA has direct control over inputs, outputs and the resources used in R&C transactions and is less reliant on third parties for direct service delivery to veterans which is consistent with the scope of this audit.
1.35 The approach ensured consideration of DVA’s significant transactional operations. The audit directly considered 56 per cent of DVA’s expenditure under Outcome 1 and Outcome 2.
1.36 The ANAO performed testing over a limited sample of R&C claims. The sample was drawn from data relating to all claims disposed from 1 October 2017 to 31 December 2017. The data was provided by DVA and included data for all R&C claim types. Details of the testing approach, including sampling is contained in Appendix 2.
1.37 The audit was conducted in accordance with ANAO auditing standards at a cost to the ANAO of approximately $365,000.
1.38 Team members for this audit were Peter Bell, Susan Ryan, Emily Urquhart, Brendon Gittins and Paul Bryant.
2. Business systems and processes
Areas examined
This chapter examines the business systems and processes that support investigation and determination of Rehabilitation and Compensation (R&C) claims. It considers the time taken to process R&C claims, how the associated workflow is managed and the impact of process design and records management on the efficiency of claims processing.
Conclusion
DVA business systems and processes have weaknesses that impact on the efficiency of claims processing, specifically in the segmented approach to processing Military, Rehabilitation and Compensation Act 2004 and Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 claims and the absence of effective workflow management over all R&C claims.
DVA’s total average TTTPs (as at February 2018) are under its internal targets, however there was no evidence of the rationale for the setting of these targets or an objective assessment of their appropriateness.
DVA’s focus on the use of the median and the average TTTP does not provide a sufficiently complete picture of performance, and does not address critical risks given that even a small number of very high TTTP claims can have significant impacts for veterans and DVA’s reputation.
Overview of Rehabilitation and Compensation business systems and processes
2.1 Claims under the Veterans’ Entitlements Act 1986 (VEA) are determined through an end-to end process that comprises:
- Registration and digitisation; and
- Investigation and determination of the claim.
2.2 For other types of claims, DVA’s processes for determination of R&C claims are separated into the following ‘modules’ based on the type of activity:
- Registration and digitisation of claims;
- processing of claims under the Military, Rehabilitation and Compensation Act 2004 (MRCA) and the Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 (DRCA), which is split between:
- investigation and determination of Initial Liability;
- Needs Assessment7;
- investigation and determination of Permanent Impairment; and/or
- investigation and determination of Incapacity.
2.3 DVA’s processing staff are specialised in handling the type of claim to which they are assigned and are generally dedicated to processing within an individual claim type.
2.4 DVA operates a national business model for the management of R&C claims. Under this model, processing of certain types of claims is carried out in prescribed locations, as shown in Table 2.1. From time to time management adjusts the flow of cases to the various locations to manage workload and the backlog of claims.
Table 2.1: Processing locations
|
|
Processing location |
||||
|
Claim Typea |
Melbourne |
Brisbane |
Perth |
Sydney |
Adelaide |
|
VEA |
✔ |
N/A |
N/A |
N/A |
N/A |
|
MRCA Initial Liability |
✔ |
N/A |
N/A |
✔ |
N/A |
|
DRCA Initial Liability |
✔ |
N/A |
N/A |
N/A |
N/A |
|
MRCA Permanent Impairment |
|
✔ |
✔ |
N/A |
N/A |
|
DRCA Permanent Impairment |
✔ |
✔ |
✔ |
N/A |
N/A |
|
MRCA/DRCA Incapacity |
N/A |
✔ |
✔ |
N/A |
✔ |
Note a: The table only includes the claim types that were subject to analysis and testing as part of this audit. Not all claim types have been included.
Source: DVA.
2.5 The determination of claims by a delegate requires an investigation of:
- the validity of the submitted claim (including proof of identity of the claimant);
- diagnosis of the claimed condition(s); and
- causality between the claimed condition(s) and the military service of the claimant.
2.6 The investigation typically requires consultation with third parties such as the Department of Defence for the medical and service records of the claimant, and with medical specialists8 for the diagnosis of claimed conditions.
2.7 Figure 2.1 provides an overview of the processes for investigation and determination of claims submitted. It distinguishes between those processes performed by DVA staff and those involving third parties.
Figure 2.1: High level outline of processes for investigation and determination of claims
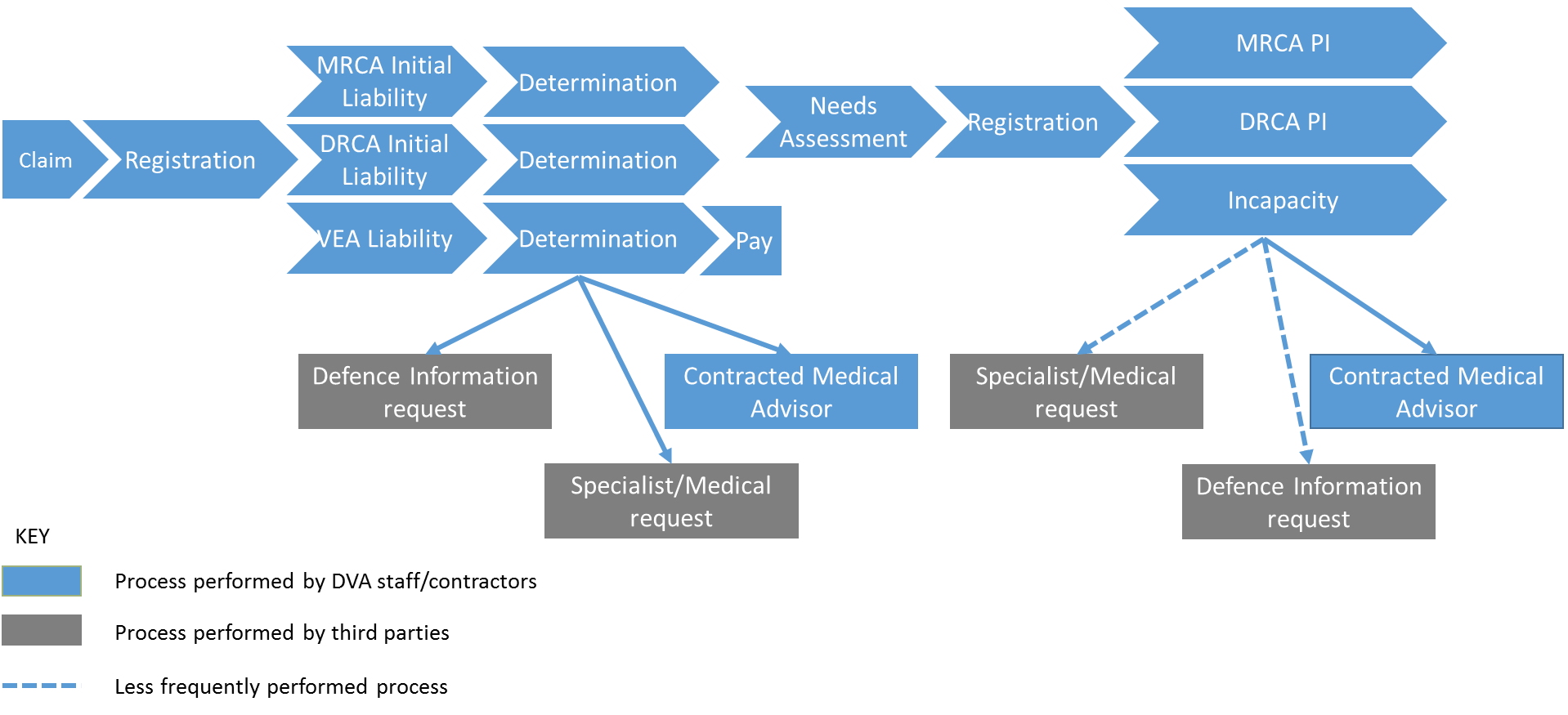
Source: ANAO analysis of DVA processes.
2.8 Differences in the legislative provisions between the Acts result in different processes and judgements being required to assess various types of claims. Two key differences are:
- DRCA legislation requires an assessment of each individual condition rather than the overall claim. On average a DRCA claim represents about three conditions. This has an impact on the efficiency of processing claims for Initial Liability and subsequently for compensation, as illustrated in Figure 2.2.
- DRCA legislation requires a ‘beyond reasonable doubt’9 level of proof, whereas VEA and MRCA legislation include provisions for a beneficial standard of proof being ‘reasonable satisfaction’ for warlike and non-warlike service. As a consequence there are higher rates of rejection for DRCA claims particularly where evidence supporting the claim is not readily available.
Figure 2.2: Illustrative DRCA process flow showing aggregation/disaggregation
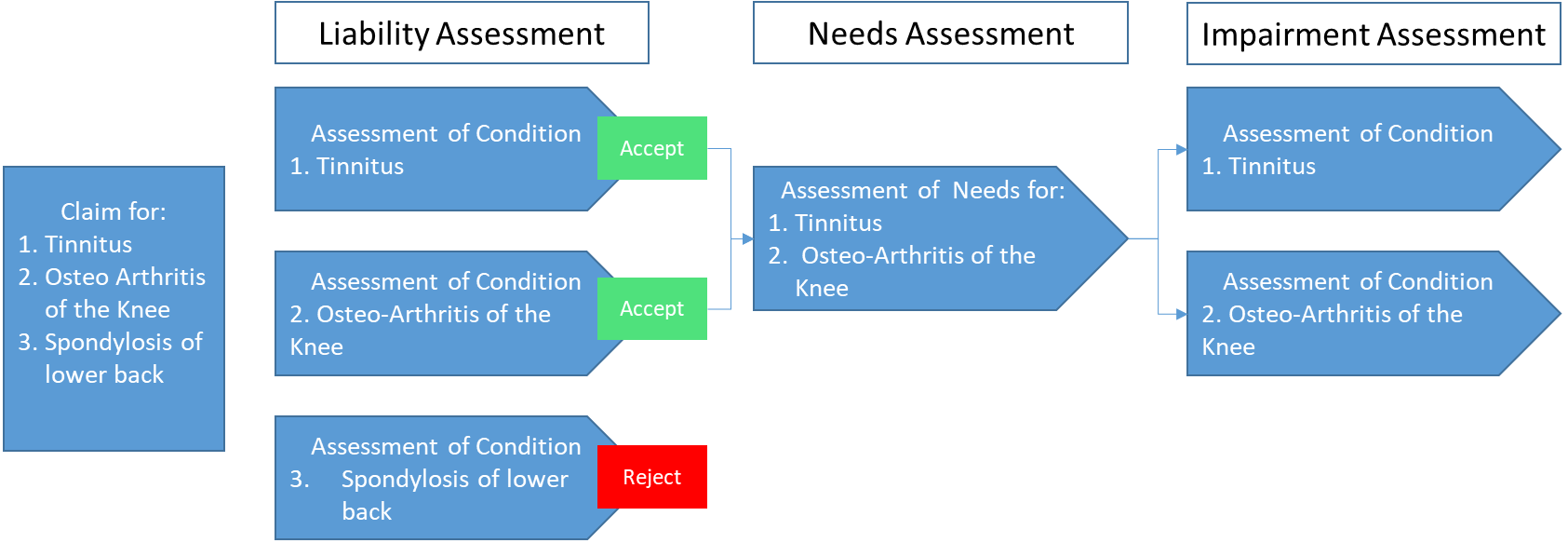
Source: ANAO analysis of DVA processes.
Is there effective workflow management of Rehabilitation and Compensation claims?
Whilst a high level workflow methodology has been established for R&C claims, the Rehabilitation and Compensation Integrated Support Hub (ISH) system is not being used to support compliance and management of workflow, but rather as a repository of records associated with a claim at the completion of processes.
ISH workflow management has been replaced in practice by individual spreadsheets maintained in various formats.
DVA’s approach to claims allocation and management means that claims can be ‘lost’ in the various hand-off points between areas, causing delays and inefficiencies.
2.9 Workflow is the sequence of processes through which a piece of work passes from initiation to completion. For R&C claims, there is a clearly understood set of high-level activities required to register, investigate and determine a claim. However, the execution of this set of activities will be impacted by the individual circumstances of the claim.
2.10 The primary system for processing R&C claims is the Rehabilitation and Compensation Integrated Support Hub (ISH). ISH has only recently been implemented for several of the claim types, and legacy systems continue to support parts of the processing. This has required DVA staff to process claims using multiple systems which could affect timeliness and accuracy of processing.
2.11 Testing identified that the workflow of R&C claims is primarily managed through the use of spreadsheets that are maintained outside of the primary processing system (ISH). The spreadsheets are developed to meet the preferences of individual team leaders and staff and there is no consistency in the workflow management within or between the types of claims processed. Spreadsheets lack formalised change/version control and reporting, increasing the risk of error. This can make spreadsheets unreliable corporate data handling tools, as accidental or deliberate changes can be made to formulae and data, without there being a record of when, by who, and what change was made.
2.12 The ISH system does not require a sequential approach to processing of claims. In practice, therefore much of the processing of claims is performed outside of ISH and the results of the processes are input into the system when they are complete.
2.13 One impact of the lack of formal workflow management is that the status of claims cannot be easily identified by management. For the whole period of processing a claim, its status is recorded in ISH as ‘under investigation’. Processing R&C claims can take substantial periods of time and management has limited information about the progress of claims or the cause of any delays.
2.14 The processing of R&C claims is modular in that the investigation of Initial Liability, the Needs Assessment and the investigation of compensation for the accepted condition(s) (Permanent Impairment or Incapacity) are conducted separately from each other (often by different teams). The modular approach was endorsed by the 2011 Review of Military Compensation Arrangements which recommended it be retained.10 The Government accepted the recommendation indicating that the approach would ‘simplify the claims process by firstly dealing with initial liability and needs assessment and then addressing claims that will satisfy the identified needs’. One advantage of the modular approach is that it allows for the application of module specific, specialist skills to less straightforward claims.
2.15 The approach adopted by DVA has resulted in the Needs Assessment process being isolated from the Initial Liability Assessment.11 This has led to more staff being involved in the processing of individual claims and the duplication of the registration and assignment of claims as they pass through the various modules.
2.16 The assignment of claims to delegates (generally through Registration on receipt of the claim or after Needs Assessment) does not lead to the routine monitoring of the progress of individual claims. DVA systems do not provide management with visibility over whether all claims registered have been directed to the correct processing area, or whether actions have been taken by delegates. As a result, misdirected claims can remain inactive until detected by either the individual assigned the claim, or the monitoring and reporting of exceptions. The ANAO observed one claim in its testing that was effectively ‘lost’ between Registration and assignment to the relevant processing area for 183 days and was not detected by governance processes.
2.17 It is the delegate’s responsibility to progress claims in a timely manner, including follow up with medical specialists and resolving any issues with the client. Although DVA statistics indicate that most claims are progressed by delegates within targets (refer Table 2.6 on page 36), there is limited transparency or control over this processing. Monitoring arrangements are focused on claims more than 240 days old and the ‘top 20’ oldest claims in the system. There is limited management visibility over claims that have not yet reached these thresholds.
2.18 The transition of claims through the various process segments is also not transparent to DVA’s clients, as evidenced in representations made to the recent Senate Inquiry into suicide by veterans.12
2.19 The lack of effective workflow management is a weakness in the system that affects both the ability for DVA to oversee the processing of claims and DVA’s efficiency in dealing with claims. These matters are further discussed in Chapter 3.
Recommendation no.1
2.20 The ANAO recommends that DVA establish appropriate workflow management over R&C processes that will allow for identification of potentially problematic claims and delays in processing earlier in the claims investigation process.
Department of Veterans’ Affairs response: Agreed.
2.21 Under the Improving Processing Systems program the Department is in the process of replacing 18 legacy systems with a single rehabilitation and compensation processing system. The new system, Rehabilitation and Compensation Integrated Support Hub (R&C ISH), will streamline claims processing and has workload management capability. While the R&C ISH currently posts tasks, it is proposed that the business area work with the IPS program to enhance active monitoring of the claims process.
2.22 The Department agrees that management controls and reporting are key areas of focus. R&C ISH improvements through future releases will include better management reporting.
2.23 In addition, R&C ISH will enable tasking and automatic alerts when key milestones are not met in the claims investigation process.
2.24 The Department has commenced work on streamlining processes and combining work efforts so the initial gathering of information can contribute to earlier processing of multiple claim types. This will result in a reduction in processing times and less duplication of effort by clients and delegates.
2.25 Furthermore, recent work with Defence aims to provide more timely access to Defence records.
Are DVA’s Rehabilitation and Compensation processes designed to maximise efficiency?
R&C processes for VEA claims are designed as an end-to-end process. However, R&C processes for DRCA and MRCA claims are not designed to maximise efficiency. The approach to assessment for these claims is resulting in the unnecessary disaggregation and re-aggregation of components within some DRCA claims, information requests to third parties being lodged multiple times for the same claims and multiple areas of DVA being required to review the same voluminous case files.
In the ANAO sample, information requests from the Department of Defence and medical specialists took a large proportion of the elapsed time taken to process (TTTP) a claim. DVA’s internal targets and external reporting for R&C claims are not well aligned to the current agreement with the Department of Defence.
2.26 VEA claims are dealt with in a singular process that encompasses Initial Liability assessment through to final payment of the claim. This section of the report is focused on arrangements for MRCA and DRCA claims that result in a claim for Permanent Impairment or Incapacity. These claims treat Initial Liability and the compensation (Permanent Impairment or Incapacity) as separate process segments.
DVA’s approach to claims processing
2.27 DVAs current approach to the processing of R&C claims isolates the assessment of Initial Liability, which considers the existence and causation of a condition, from the subsequent assessment of the claim for rehabilitation or compensation for the condition. This is resulting in the duplication of some processes and instances of substantial delay for clients. For example, a medical assessment that is sufficient for a delegate to accept Initial Liability for a condition may not be appropriate for the investigation of Permanent Impairment (permanency, stability and degree of the condition). This is best illustrated by the following example:
2.28 A claim of a ‘sprain’ (a temporary condition) may be acceptable for an Initial Liability assessment but would not be acceptable for Permanent Impairment assessment if that was the result of a client’s Needs Assessment. In this case, an assessment of joint instability (a permanent condition) would be more appropriate. Both diagnoses may be correct, but a diagnosis of joint instability would serve both Initial Liability and Permanent Impairment assessments. Where the Initial Liability diagnosis of a ‘sprain’ has been accepted for a client seeking Permanent Impairment compensation, a repeat Initial Liability assessment is required that may require an additional medical consultation. This would result in a delay in the compensation payment and frustration for the veteran.
2.29 DVA’s approach to processing also means that the individual processing modules may not be consistently incentivised. For example, the targets for Initial Liability assessment are explicitly time based for that module (they are based on the TTTP). This fails to recognise that a more comprehensive assessment of Initial Liability could result in a more straightforward and faster Permanent Impairment or Incapacity assessment and payment. For example, extending the time taken for the Initial Liability assessment by including a more comprehensive medical diagnosis covering not only Initial Liability requirements, but also those of Permanent Impairment or Incapacity could result in improved timeliness of end-to-end claims processing.
2.30 The ANAO observed, during fieldwork, two claims where the investigation conducted for determination of Initial Liability was deemed insufficient by the delegate to support the subsequent Permanent Impairment investigation. In these two cases, had the Initial Liability delegate considered the potential Permanent Impairment claim, a different diagnosis would have been sought. This meant that for both claims additional medical advice was needed resulting in delays in processing.
2.31 The following table summarises the waiting times for responses to requests for information from medical specialists across the four modules of high TTTP claims in the ANAO’s testing. The table shows that there are periods of waiting both for the Initial Liability and at the subsequent Permanent Impairment modules, but that the Permanent Impairment module waiting times are higher.
Table 2.2: Analysis of waiting time by module for medical information in high time taken to process claims
|
Claim Module |
Waiting on Medical Specialist (average number of days) |
|
MRCA Initial Liability |
71 |
|
DRCA Initial Liability |
109 |
|
MRCA Permanent Impairment |
214 |
|
DRCA Permanent Impairment |
172 |
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 and 31 December 2017.
2.32 Typically, the assessment of an R&C claim involves collection and review of several thousand pages of documentation. One impact of the DVA’s approach is that more individuals are required to read and understand a client’s claim and circumstances than under an end-to-end process. ANAO testing indicated that in at least 10 per cent of claims at least six people were required to read and understand the client’s records. This approach incurs a cost in staff time and contributes to delays in the finalisation of claims. The number of people required to read documentation is primarily impacted by two factors:
- the number of hand-offs within the process; and
- whether or not DVA procedures require case coordination (for complex/high risk claims).
2.33 A requirement of DRCA legislation is that claims are assessed as individual conditions. For example, where a single claim covers two conditions, such as Osteoarthritis of the knee and Spondylosis of the lower back, they must be considered as separate claims, even if both were caused by the same incident. Under the DVA’s current approach this means that a DRCA claim is:
- disaggregated for assessment of Initial Liability; then
- re-aggregated for Needs Assessment; and then
- disaggregated for assessment of Permanent Impairment or Incapacity.
2.34 The aggregation and disaggregation of claims is a manual process that introduces risk to the accuracy of recorded information and requires staff with experience and attention to detail. This is shown in Figure 2.2: Illustrative DRCA process flow showing aggregation/disaggregation.
2.35 One reason for the re-aggregation of DRCA claims is that the Needs Assessment requires an holistic approach to the claim, which may involve assessment of medical, vocational and psycho-social aspects. DVA is currently piloting the conduct of the Needs Assessment before the Initial Liability Assessment. This will reduce the requirement for disaggregating and re-aggregating DRCA claims. The ‘front-ending’ of the Needs Assessment will not be appropriate for all claims and individual circumstances will be relevant to how claims are processed and the timing of the Needs Assessment.
2.36 DVA has also begun the introduction of different processing requirements for the Initial Liability investigation of mental health claims and some other claims relating to, for example, sexual and physical assault. The main difference is that communication with the client is conducted by trained case coordinators rather than the delegate conducting the investigation. Testing identified that this has had the effect of increasing the time taken to complete the investigation and make a determination.
2.37 The process for assessment will frequently need to take into account a range of individual circumstances that will require flexibility in processing and judgement in reaching the appropriate determination. There will be many occasions when DVA’s current approach is in the best interest of the client. However, this approach has risks and costs that should be recognised and minimised in DVA processes.
Information requests
2.38 The investigation of claims, particularly for Initial Liability assessment, requires access to Department of Defence service and medical records. DVA and the Department of Defence have established arrangements through the use of a Single Access Mechanism (SAM) to channel and manage requests and responses for information. Oversight of DVA and Department of Defence SAMs is through the Defence/DVA Links Steering Committee (DLSC). This Committee has responsibility for agreeing key performance indicators for the SAM. At its meeting on 15 August 2017 the Committee agreed to the following key performance indicators.
Table 2.3: Key performance indicators for the Single Access Mechanism
|
Priority |
Within 12 Months of Separation |
Between 1 to 3 years from Separation |
3+ years of Separation |
|
Urgent (General) |
5 business days |
10 business days |
15 business days |
|
Urgent (Complex) |
20 business days |
20 business days |
30 business days |
|
Medium |
15 business days |
20 business days |
25 business days |
|
Routine |
25 business days |
30 business days |
35 business days |
Source: Defence/DVA Links Steering Committee.
2.39 As outlined above, the nature of the agreement with Department of Defence includes factors such as the urgency and the length of separation from Defence. In contrast the DVA’s performance measures are focused on a single metric, the TTTP.13
2.40 In Table 2.4 below, the agreed response times for information requests from the Department of Defence are shown as a percentage of the TTTP target DVA has established for Initial Liability assessments of VEA and MRCA/DRCA claims. This indicates, for example, that the response time for ‘routine’ priority cases for veterans with greater than three years separation from the Australian Defence Force (ADF) equates to 65 per cent of the TTTP target for VEA claims (75 days) and 40 per cent of the TTTP target for MRCA/DRCA claims (240 days). It is important to note that the SAM targets are expressed in business days and the DVA TTTP is expressed in calendar days.
Table 2.4: Performance indicator for the Single Access Mechanism to respond to information requests
|
|
VEA – TTTP Target days 75 |
MRCA/DRCA – TTTP Target days 120 |
||||
|
Priority |
Within 12 months of Separation |
Between 1 to 3 years from Separation |
3+ years of Separation |
Within 12 months of Separation |
Between 1 to 3 years from Separation |
3+ years of Separation |
|
Urgent (General) |
9.3% |
18.7% |
28.0% |
5.8% |
11.7% |
17.5% |
|
Urgent (Complex) |
37.3% |
37.3% |
56.0% |
23.3% |
23.3% |
35.0% |
|
Medium |
28.0% |
37.3% |
46.7% |
17.5% |
23.3% |
29.2% |
|
Routine |
46.7% |
56.0% |
65.3% |
29.2% |
35.0% |
40.8% |
Source: ANAO analysis of SAM performance indicators.
2.41 The DVA TTTP target approach is therefore insufficiently aligned to the targets under the SAM agreement. This misalignment in approach means that there will be greater variability around the single metric target adopted by DVA.
2.42 A high proportion of claims assessed for Initial Lability will also require advice from a medical specialist to provide an acceptable diagnosis of the condition claimed. ANAO testing indicated the average amount of time required for diagnosis of claimed medical conditions was 150 days for the 53 high TTTP claims examined. This time is not representative of all claims. However, it is an indicator that this activity can, and does, lead to claims taking longer than target for TTTP. This is illustrated in Table 2.5 below.
Table 2.5: Time waiting for advice from medical specialists in high time taken to process claims sampled
|
|
Sample results for High TTTP |
||||
|
Claim type |
Average TTTP |
Target |
Waiting on medical specialists |
% of average TTTP spent waiting on medical specialists |
% of target time attributable to waiting on medical specialists |
|
VEA |
393 |
75 |
185 |
47 |
247 |
|
MRCA Initial Liability |
366 |
120 |
71 |
19 |
59 |
|
DRCA Initial Liability |
428 |
120 |
109 |
25 |
91 |
|
MRCA Permanent Impairment |
322 |
120 |
214 |
66 |
178 |
|
DRCA Permanent Impairment |
350 |
120 |
172 |
49 |
143 |
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 and 31 December 2017.
2.43 The time taken to access information from the Department of Defence and from medical specialists constitutes a major component of the overall time taken to process a claim. DVA should ensure that irrespective of its approach to systems and processing, that the number of requests for information from third parties is the minimum necessary to effectively deal with the claim.
Recommendation no.2
2.44 The ANAO recommends that DVA review the current approach to processing R&C claims to address efficiency issues including aggregation and disaggregation of DRCA claims, multiple instances of information requests to third parties and the number of staff involved in the processing of individual claims.
Department of Veterans’ Affairs response: Agreed.
2.45 Historically, the processing systems had been developed to support processing in the administration of the various individual pieces of legislation. This has influenced organisational design and the Department’s approach to processing claims. With the development of a single processing system the Department is well placed to examine the existing claims process and practices.
2.46 The Department is developing changes to team design and workflow, drawing on the risk and client population segmentation analysis (collected through the Veteran Centric Reform) to prospectively manage the claim and client through a single point of contact for all Initial Liability (IL) claims. This work is in the very early stages and builds on improved capability brought by the ISH.
2.47 Needs Assessments are now done at the beginning of the IL claims process. This could identify cases where IL and Incapacity or Permanent Impairment (PI) could be processed concurrently in the future.
2.48 The work on the medical forms to include IL and PI questions also has the potential to reduce the number of separate medical visits for diagnosis and assessment.
What metrics are being used to measure Rehabilitation and Compensation efficiency, and are these appropriate?
DVA focuses on the median and the mean time taken to process (TTTP) in both operational and external reporting for the performance of the Rehabilitation and Compensation (R&C) business. Reporting indicates that the average TTTP, number of cases-on-hand, and average age of cases fell across all R&C claim categories in the period 2015 to 2017.
Total average (mean) TTTPs (as at February 2018) are under DVA’s targets of 90 days (VEA) and 240 days (MRCA and DRCA) for end-to-end processing. There was no evidence of the rationale for the setting of the TTTP targets or an objective assessment of the appropriateness of the target times.
DVA’s focus on the use of the median and the average TTTP does not provide a sufficiently complete picture of performance as it does not necessarily address critical risks given that even a small number of very high TTTP claims can have significant impacts for veterans and DVA’s reputation.
2.49 DVA prepares regular reports that include information about the TTTP within the processing modules to track performance across all of DVA’s R&C processes. The reports for the period February 2017 to February 2018 focus on the median and average TTTP and indicate an improving trend. This is illustrated in Figure 2.3, the selected modules of which are broadly representative of the R&C business operations as a whole. Additional Information is included in Appendix 3.
Figure 2.3: Extract from DVA national reporting of median and trend information for disposed claims February 2017 to February 2018
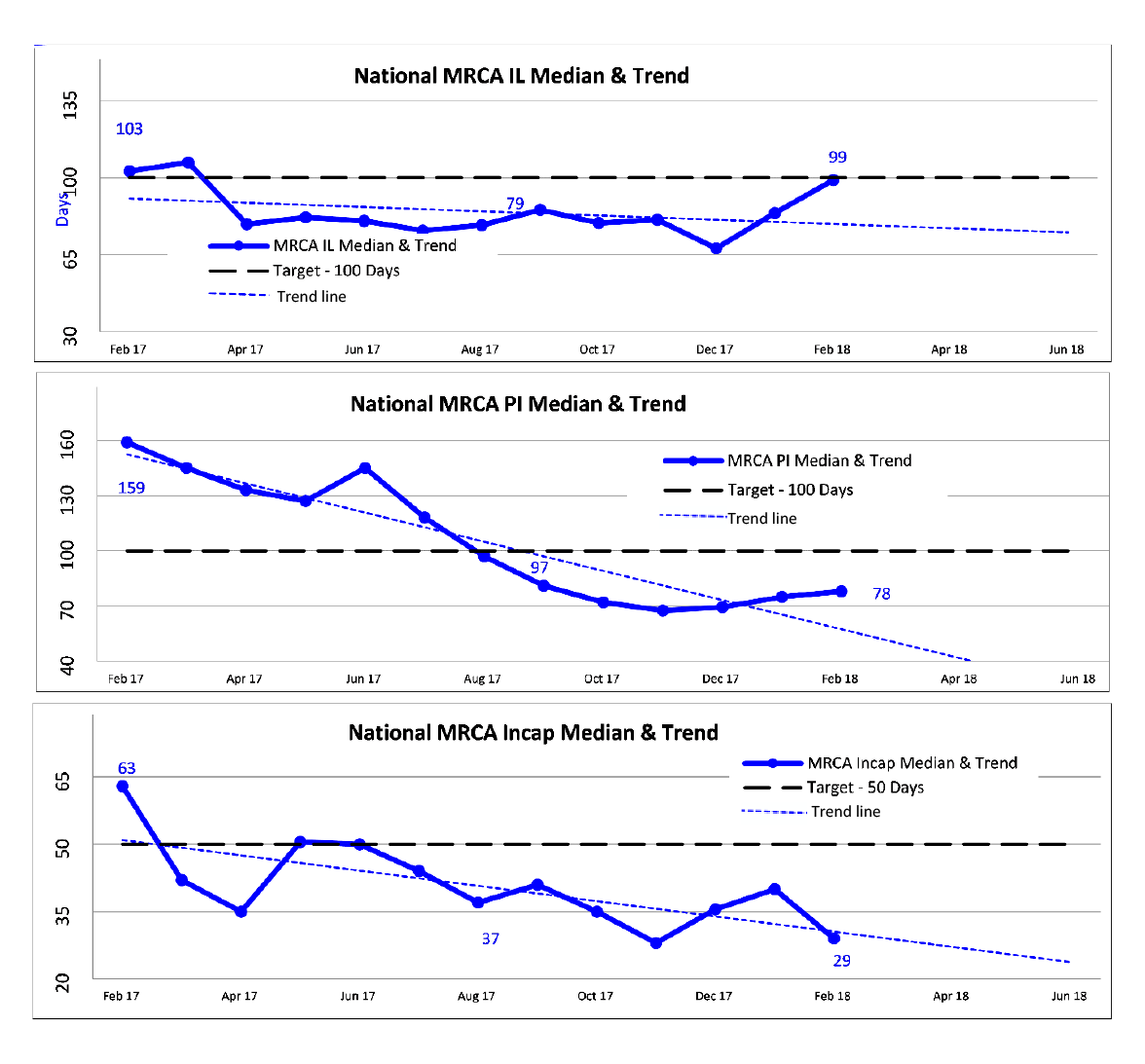
Notes: ‘IL’ – Initial Liability claim. ‘PI’ – Permanent Impairment claim. ‘Incap’ – Incapacity claim.
Source: DVA Rehabilitation & Compensation National Reporting.
2.50 Table 2.6 shows the change in the average TTTP for finalised claims between 2015-16 and 2016-17 across a number of claim types.
Table 2.6: Average time taken to process for finalised claims (in days)
|
|
|
Number of days |
Change since last financial year |
||
|
Claim Type / Module |
Target |
2015-16 |
2016-17 |
Number of days |
% |
|
VEA |
75 |
72 |
72 |
0 |
0.0 |
|
MRCA Initial Liability |
120 |
117 |
107 |
-10 |
-8.5 |
|
DRCA Initial Liability |
120 |
118 |
110 |
-8 |
-6.8 |
|
MRCA Permanent Impairment |
120 |
161 |
156 |
-5 |
-3.1 |
|
DRCA Permanent Impairment |
120 |
163 |
148 |
-15 |
-9.2 |
|
MRCA/DRCA Incapacity |
90 |
87 |
81 |
-6 |
-6.9 |
Source: DVA claims statistics.
2.51 Overall, DVA reporting shows that the average TTTP has reduced for every claim type except for VEA, where it has remained constant. Despite this overall reduction, the average TTTP for MRCA and DRCA Permanent Impairment in 2016-17 is above target, indicating that processing times for these categories are not being achieved. Since June 2017, management reporting indicates a positive trend into 2017-18, and that at February 2018 all claim types were under target for TTTP.
2.52 The number of cases-on-hand is an indicator of the work-in-progress in R&C claims in DVA. The table below illustrates the number of cases-on-hand at a point in time, and indicates that there was a reduction in the number of cases-on-hand of 17.9 per cent across all processing elements between 2015-16 and 2016-17.
Table 2.7: Cases-on-hand
|
|
Number of cases |
Change since last financial year |
||
|
Claim Type / Module |
2015-16 |
2016-17 |
Number of cases |
% |
|
VEA |
3,544 |
2,549 |
-995 |
-28.08 |
|
MRCA Initial Liability |
2,584 |
2,314 |
-270 |
-10.45 |
|
DRCA Initial Liability |
2,133 |
1,822 |
-311 |
-14.58 |
|
MRCA Permanent Impairment |
2,008 |
1,988 |
-20 |
-1.00 |
|
DRCA Permanent Impairment |
1,938 |
1,370 |
-568 |
-29.31 |
|
MRCA/DRCA Incapacity |
452 |
350 |
-102 |
-22.57 |
|
Total |
12,659 |
10,393 |
-2,266 |
-17.90 |
Source: DVA Rehabilitation & Compensation National Reporting.
2.53 The average age of cases-on-hand is an indicator of the backlog of work in R&C. The table below illustrates that between 2015-16 and 2016-17 there was a reduction in the average age of cases on hand of 188 days or 29.1 per cent.
Table 2.8: Average age of cases on hand (in days)
|
|
Number of days |
Change since last financial year |
||
|
Claim Type |
2015-16 |
2016-17 |
Number of days |
% |
|
VEA |
93 |
70 |
-23 |
-24.73% |
|
MRCA Initial Liability |
103 |
66 |
-37 |
-35.92% |
|
DRCA Initial Liability |
129 |
82 |
-47 |
-36.43% |
|
MRCA Permanent Impairment |
119 |
100 |
-19 |
-15.97% |
|
DRCA Permanent Impairment |
111 |
90 |
-21 |
-18.92% |
|
MRCA/DRCA Incapacity |
91 |
50 |
-41 |
-45.05% |
Source: DVA Rehabilitation & Compensation National Reporting.
2.54 The TTTP is intended to provide a measure of the time between receipt of a claim and determination by a delegate or withdrawal by the client. The following table illustrates the average TTTP by process step for Permanent Impairment claims at February 2018.
Table 2.9: Average end-to-end time taken to process Permanent Impairment claims as at February 2018
|
Process step |
Days to process |
|
|
|
MRCA |
DRCA |
|
Registration* |
1 |
1 |
|
Initial Liability Assessment |
88 |
92 |
|
Needs Assessmenta |
10 |
10 |
|
Registration* |
1 |
1 |
|
Permanent Impairment Assessment |
90 |
87 |
|
Total |
190 |
191 |
Note a: The number of days for Registration and Needs Assessment are estimates as this information is not included in DVA management reports.
Source: DVA Rehabilitation & Compensation National Reporting.
2.55 The total average TTTPs in the table above are under DVA’s targets of 240 days (MRCA) and 240 days (DRCA) for end-to-end processing. However, there was no evidence of the rationale for the setting of the TTTP targets or an objective assessment of the appropriateness of the target times.
2.56 DVA’s primary focus in external reporting of claims performance was the average (mean) TTTP but more recently has been the median14 TTTP.15
2.57 At an operational level, team leaders who directly manage delegates focus explicitly on the average TTTP.
2.58 The average TTTP is calculated by dividing the TTTP for all claims by the total number of claims. For the purposes of calculating the average, DVA ignores claims processed in 0 days. The median expresses the TTTP for DVA to dispose of 50 per cent of its claims in ‘X’ number of days.
2.59 ANAO analysis of claims with a low TTTP processed between 1 October 2017 and 31 December 2017 indicates that many of the claims with a TTTP of 1 day do not reflect claims that are representative of ‘normal’ claims processing. For example, they are frequently Veterans’ Review Board or Administrative Appeals Tribunal referrals of set aside decisions and require no formal investigation. The inclusion of these claims distorts both the median and average TTTP.
2.60 The ANAO also analysed two claims with a TTTP of less than five days (but not 0 or 1 days). Whilst this analysis is not representative of the entire population, it indicated claims which did not reflect ‘normal’ processing. The analysis found misrecording of processing module dates and claim activities for part determinations and sequelae16 which do not require complete processing.
2.61 For the total population R&C claims disposed between 1 October 2017 and 31 December 2017, the median was less than the average. This indicates that a large number of claims were processed relatively quickly, resulting in a distribution curve that shows that 50 per cent of claims were processed in less than 70 days but that the remaining 50 per cent took between 71 and 480 days. This confirms that DVA has a ‘tail’ of long standing claims, as illustrated in Figure 2.4.
Figure 2.4: Typical distribution of the various processing modules
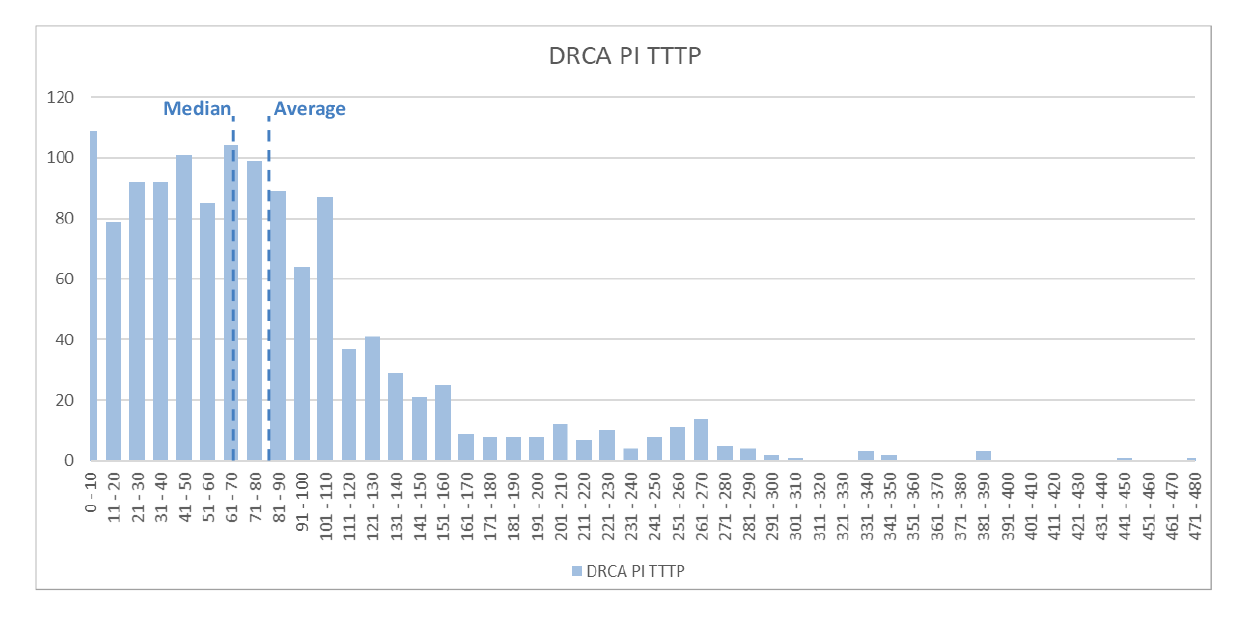
Source: ANAO analysis of claims finalised between 1 October 2017 and 31 December 2017.
2.62 The overall population of data for claims disposed between 1 October 2017 and 31 December 2017 indicates that 158 claims older than 240 days were disposed during the period, which equates to 1.8 per cent of total claims disposed over this time.17
2.63 The average and/or median TTTP for R&C claims are not complete indicators of DVA’s efficiency in processing claims. The variability of the TTTP for claims disposed between 1 October 2017 and 31 December 2017 was significant, as illustrated in Figure 2.4 above and Table 2.10.
Table 2.10: Analysis of variability in time taken to process 1 October 2017 to 31 December 2017
|
Module |
Minimum TTTPa |
Median |
Average |
Maximum TTTP |
|
VEA |
1 |
96 |
112 |
406 |
|
MRCA Initial Liability |
1 |
84 |
88 |
619 |
|
DRCA Initial Liability |
1 |
71 |
84 |
365 |
|
MRCA Permanent Impairment |
1 |
84 |
86 |
433 |
|
DRCA Permanent Impairment |
1 |
69 |
81 |
477 |
|
MRCA Incapacity |
1 |
35 |
40 |
163 |
|
DRCA Incapacity |
1 |
30 |
41 |
176 |
Note a: When preparing performance information the DVA removes the claims with 0 days. Claims with 1 day or more are included in the measurement of median.
Source: ANAO analysis of claims finalised between 1 October 2017 and 31 December 2017.
2.64 The Standard Deviation of the DRCA Permanent Impairment data for claims disposed between 1 October 2017 and 31 December 2017 is 66 days, indicating a wide distribution in the data set. This is consistent with the ANAO’s observation that the use of the average and median as indicators of performance without consideration of the wide distribution of TTTP of claims provides an incomplete view of performance. A measure representing the top 5 percentile taking longer than a period of ‘X’ days would provide a more valuable insight into the claims with high TTTPs and enable DVA to direct its attention to those claims. This information can be drawn from existing management reports, but is not a focus of these reports. A broader measure than the median TTTP would enable management to focus more closely on potentially problematic claims.
Recommendation no.3
2.65 The ANAO recommends that DVA implement claims processing targets that include consideration of the distribution of the TTTP as well as the average/median.
Department of Veterans’ Affairs response: Agreed.
2.66 The Department has a number of processing targets for compensation claims which are included in the monthly performance report. The performance reports are regularly reviewed to monitor and manage claims performance and the age profile of on hand workloads.
2.67 These targets are currently being reassessed to align them with the median targets and the monthly reports will progressively be updated once there is sufficient data.
2.68 In addition, a comprehensive weekly report is produced to show the age analysis of work on hand by function and by location. This report plus clarity about SES and line management responsibility and accountability for the various components of R&C business will allow for improvements to the overall management of claims processing targets.
2.69 Furthermore, recent work with Defence aims to provide more timely access to Defence records.
2.70 The Department will examine the feasibility of extending the range of reports available, including the distribution of TTTP, to monitor and manage claims processing.
Does DVA information and records management adequately support decision making?
Testing identified inconsistencies in naming conventions for records in ISH and HP Content Manager, DVA’s primary records management system. Locating all relevant documentation associated with a claim during the testing process was inefficient and time consuming.
It is apparent that the ISH system does not have controls to ensure integrity over the high volume of manual records placed in the system. This was particularly evident in relation to the dates associated with registration of claims and referral for medical consultations. Instances were also identified where key client documentation was being kept manually by staff for periods prior to lodgement in the ISH system.
2.71 A single claim for a client typically results in the creation of many thousands of pages of records. As DVA has a long term relationship with the majority of its clients, it is common for each client to have multiple claims recorded. The ability to find complete and accurate records is an important efficiency and service delivery consideration. It is especially important that DVA is able to locate critical information such as service and medical records to avoid unnecessary and time consuming information requests.
2.72 DVA uses HP Content Manager as its primary records management system. This system is linked to ISH and is the primary information repository for R&C processing.
2.73 In preparing the chronologies for the high TTTP claims tested by the ANAO, specific information about the timing of information requests and the subsequent return of information was identified and recorded. There were 16 instances from a sample of 53 where either a response was received without a request on file, or a request was on file without a corresponding receipt of information being recorded, even though a determination was made.
2.74 ISH does not automatically generate documents with titles that follow DVA document naming conventions. Similarly, staff are able to store records in HP Content Manager without following required naming conventions. Testing noted high levels of inconsistency in the naming of individual claim records. Under the current arrangements it is time consuming to locate relevant records and there is frequent uncertainty whether all relevant records have been found.
2.75 The examination of client records in the high TTTP claims testing identified instances where incorrect dates had been recorded. For example, where the claims received date was inaccurate and did not reflect attached supporting documentation. There were similar inconsistencies in other dates such as the recording of withdrawal and determination dates. In one instance, there was an email that had been filed on HP Content Manager that contained attachments which were dated after the sent date in the email. There is no facility within ISH that either prevents or flags when key dates have been changed. ANAO analysis of the sample of 10 MRCA Initial Liability and 10 MRCA Permanent Impairment cases (for dates of receipt and dates of determinations) identified 14 incorrectly recorded dates.
2.76 Testing further indicated instances where information emailed directly to DVA staff was not uploaded into HP Content Manager in a timely manner. There is no systemic control over the completeness of records included in official records management systems.
2.77 There are risks for DVA in incomplete or inaccurate records for its clients as this can directly lead to inefficiency, inaccuracy or a lack of timeliness in service delivery.
Recommendation no.4
2.78 The ANAO recommends that DVA addresses weaknesses in information and records management, in particular: retention of records outside of primary systems, inconsistent use of naming conventions, and ensuring the completeness and accuracy of client records.
Department of Veterans’ Affairs response: Agreed.
2.79 A program of work to implement an overarching quality strategy to improve information and records management is to be developed. This will build on the work undertaken by the Quality Assurance process to identify systemic, competency, and behavioural issues leading to weaknesses in information and record management. The overarching quality strategy will also incorporate analysis of client feedback.
3. Delivery of services
Areas examined
This chapter examines measures of efficiency for DVA’s processing of Rehabilitation and Compensation (R&C) claims. It focuses on the time taken to process (TTTP) and categorises activities through the use of case chronologies for a sample of R&C claims. It also examines transparency and reporting to identify whether management information supports governance and oversight of claims. This chapter also examines DVA’s staffing model for the processing of claims.
Conclusion
DVA can improve the efficiency of high TTTP claims processing by reducing the amount of ‘inactivity’ (delays in the actioning of a claim despite the presence of required information) and through the more structured management of medical specialists.
The monitoring and reporting of claims is not effective in alerting management to those which are at risk of taking excessive time to process.
What are the key drivers behind claims with a high time taken to process?
Testing indicated that the two main drivers of high TTTP claims were the need to wait for responses from medical specialists, and ‘inactivity’.
Unlike the Single Access Mechanism (SAM) arrangements with the Department of Defence, there is no formal control or monitoring of requests for information from medical specialists. Time spent waiting for responses from medical specialists in the ANAO’s testing was, on average, 10 times greater than for information requests to the Department of Defence.
There were two main reasons for ‘inactivity’: where claims were effectively ‘lost’ in the system, and where the delegate did not immediately take action after requested information was received and the claim was actionable. Both issues are indicative of a lack of transparency over workflow within the system.
Analysis of efficiency in the sample of high time taken to process cases
3.1 A typical R&C claim (other than Veterans’ Entitlements Act 1986 (VEA)) at February 2018 took more than 190 days to process from end-to-end.
3.2 ANAO analysis of 53 high time taken to process (TTTP) claims was focused on identifying characteristics that caused the high TTTP. The claims were sampled from VEA, Military, Rehabilitation and Compensation Act 2004 (MRCA) and Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 (DRCA) claims disposed between 1 October 2017 and 31 December 2017. For each of the claims tested, a claim chronology or ‘clock’ was developed that categorised the time spent processing the claim. The categories were:
- active time - where DVA was engaged in progressing the claim;
- waiting time - where a request for information to the Department of Defence, to a medical specialist or to the client had been lodged and no further action could be undertaken until the information was received; and
- inactive time – where there was no evidence of activity on the claim for a continuous period of 14 days or more. This 14 day period was used to take into account off-line activities such as reading documents and preparing submissions that were not evident in the processing system. In its treatment of the sample, the ANAO classified the first 14 days of any period of apparent inactivity as ‘active’ time in order to allow for this.
3.3 The categorisation of time reflects the information that was available in the client file. If processes were performed and the documents not saved appropriately they were not reflected in the analysis. The categorisation also only reflects the 53 claims reviewed by the ANAO, which were deliberately selected with a bias toward claims that had the highest TTTP (and will therefore not be representative of all claims).
3.4 The sample of high TTTP claims frequently included:
- claims under multiple Acts;
- claimants overseas where, typically, medical appointments are difficult and time consuming to organise;
- claimants with complex conditions such as mental health and related conditions; and
- claimants with conditions that have arisen from historical incidents and military service.
3.5 ANAO analysis confirms that these factors lead to longer TTTP as they may result in more correspondence with the client, more consultation with medical specialists (waiting time) and may require more investigation and processing by DVA staff (active time). Inactive time in a claim’s processing is unlikely to be affected by these factors.
3.6 The breakdown of time between the categories for the claims reviewed is shown in Figure 3.1 below.
Figure 3.1: Summary of categorisation of activities on claims with high time taken to process
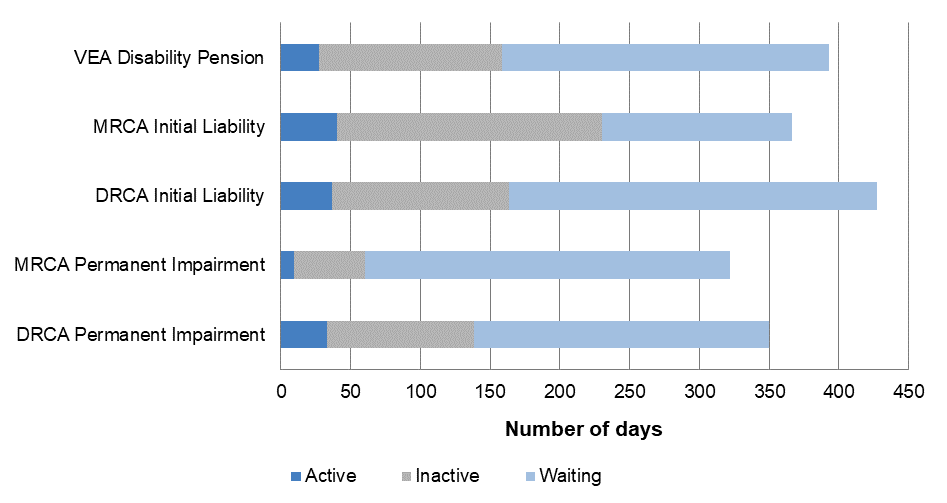
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 and 31 December 2017.
3.7 Analysis indicates that in the high TTTP claims reviewed, more than half of the processing time comprised waiting for responses from Department of Defence, medical specialists, Contracted Medical Advisors (CMA) or the client. The average time spent ‘waiting’ across the sample was 221 days out of a total average processing time of 371 days or 60 per cent of the TTTP.
3.8 In Figure 3.2 below, waiting time is analysed in more detail to show time spent waiting on the stakeholders identified above.
Figure 3.2: Analysis of activity in percentages for claims with high time taken to process
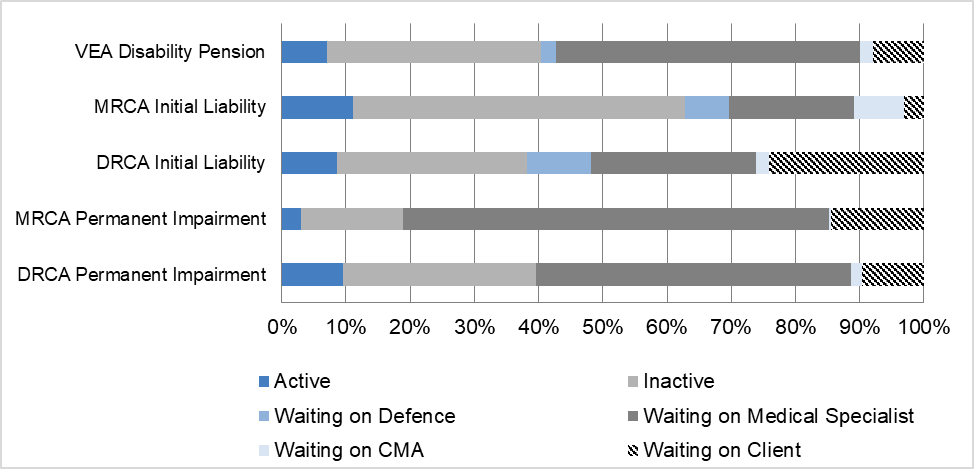
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 to and December 2017.
Medical Specialists
3.9 Analysis indicates that approximately two thirds of waiting time in the ANAO reviewed claims was attributable to obtaining information and/or advice from medical specialists. A particular contributor to long waiting times was where clients had a preference for the use of their own treating medical specialist rather than the use of a DVA referred independent medical specialist. Treating medical specialists may be unable or unwilling to provide the necessary advice and, in this situation, the time waiting for a response from the client’s treating medical specialist is wasted as further medical advice must be sought from an independent medical specialist. Two instances were identified in the ANAO reviewed claims where 222 and 163 days were respectively spent waiting for responses from treating medical specialists before referral to independent medical specialists.
3.10 Information requests from the Department of Defence through the Single Access Mechanism (SAM) and from medical specialists can be done in parallel. Detailed review of the high TTTP claims found that, requests for medical diagnoses and for Department of Defence information were not made in parallel but were conducted sequentially. This had a negative impact on the TTTP for the claim.
3.11 Staff can set resubmit reminders within the Integrated Support Hub (ISH) to flag when follow up actions are required. The timing of follow up activity is discretionary and DVA has not provided guidance to delegates on acceptable times. The ANAO observed an inconsistent approach to the follow up of information requests. The time allowed for responses from medical specialists varied significantly between delegates as did the frequency of follow up activities.
3.12 The three primary reasons why waiting time was high in the cases above were: non-responsiveness of the third party, multiple requests to third parties and/or that information received did not meet DVA requirements. The speed and frequency of DVA follow up of information requests was also a factor that contributed to longer waiting times.
3.13 The control and attention by DVA over requests for information from the Department of Defence is relatively high. This includes the use of the SAM, key performance indicators and a dedicated team for follow up and administration of the requests. On the other hand, there is no formal control or monitoring of requests for information from medical specialists. There are no formal contractual arrangements with medical specialists, including the independent medical specialists that DVA engages directly. As illustrated in Figure 3.2, the time spent waiting for responses from medical specialists is on average 10 times greater than for information requests to Department of Defence. Whilst control over information requests from medical specialists may be more difficult, it also has the potential for greater efficiencies.
Inactivity
3.14 In the high TTTP claims reviewed by the ANAO inactivity accounted for, on average, approximately one third of the TTTP. Two main reasons for these high levels of inactivity were identified: where claims were effectively ‘lost’ in the system; and where there was a delay by the delegate in taking action after requested information was received that made the claim actionable.
3.15 The effect of claims lost in the system can be substantial. In the claims reviewed, one claim was received on 22 December 2016 but was not registered, or assigned to a delegate, until 23 June 2017 − a delay of 183 days before any processing commenced. As indicated in Chapter 2, there is no systemic control to identify claims lost in this way.
3.16 Table 3.1 below summarises 10 cases from the ANAO reviewed claims where there was inactivity immediately after a claim was received or registered. For these claims, taking immediate action would have represented an efficiency improvement in the TTTP.
Table 3.1: Reviewed claims – instances of inactivity at the beginning of processing
|
|
|
Inactivity at the beginning of a claim |
|
|
Claim type |
TTTP |
Days inactivea |
% of inactive time before recorded activity |
|
VEA Disability Pension Case 1 |
331 |
98 |
30 |
|
MRCA Initial Liability Case 1 |
341 |
169 |
50 |
|
MRCA Permanent Impairment Case 1 |
442 |
73 |
17 |
|
MRCA Permanent Impairment Case 2 |
378 |
53 |
14 |
|
MRCA Permanent Impairment Case 3 |
340 |
74 |
22 |
|
MRCA Permanent Impairment Case 4 |
365 |
78 |
21 |
|
MRCA Permanent Impairment Case 5 |
290 |
57 |
20 |
|
MRCA Permanent Impairment Case 6 |
288 |
43 |
15 |
|
DRCA Permanent Impairment Case 1 |
336 |
134 |
40 |
|
DRCA Permanent Impairment Case 2 |
387 |
129 |
33 |
Note a: These figures exclude the 14 days of assumed ‘active’ time for each period of inactivity.
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 and 31 December 2017.
3.17 Inactivity in claims occurs throughout the lifecycle of a claim and is frequently comprised of a series of periods of inaction between processing steps. For example, in one claim reviewed a period of 66 days elapsed between assignment to a delegate and an initial request for medical information. There was no activity recorded in the file for this period. Later, for the same claim, there was an 82 day period where no activity was recorded between receipt of the medical information and the request for the impairment assessment from the CMA. In effect, the claim appears to have taken 148 days longer to process than would have been the case had action been taken expeditiously.
3.18 From the claims reviewed by the ANAO, five instances were identified where taking immediate action after all information was received would have resulted in an earlier determination and reduced the TTTP, as shown in Table 3.2.
Table 3.2: Reviewed claims – results for inactivity after all information received
|
Claim type |
Number of days of inactivity before making a determination |
|
VEA Disability Pension Case 1 |
26 |
|
MRCA Initial Liability Case 1 |
168 |
|
DRCA Initial Liability Case 1 |
157 |
|
DRCA Permanent Impairment Case 1 |
50 |
|
DRCA Permanent Impairment Case 2 |
28 |
Source: ANAO analysis of a sample of DVA claims disposed between 1 October 2017 and 31 December 2017.
3.19 The combination of high levels of individual delegate control over the progress of cases and the limited ability to systemically identify problematic cases exposes DVA to risk. Whilst a majority of cases are dealt with expeditiously, there is limited capacity to prevent or detect high consequence events associated with high TTTP claims.
3.20 The issues of inactivity resulting in delays in processing and potentially problematic claims should be addressed through improved workflow management, which is the subject of Recommendation No.1.
Recommendation no.5
3.21 The ANAO recommends that DVA implement greater control and monitoring over its requirement for information from medical specialists. This should include contractual arrangements that prescribe timeliness and quality for independent medical specialists engaged directly by the DVA and prompt and frequent follow up where the client has elected to use their own treating medical specialist.
Department of Veterans’ Affairs response: Agreed.
3.22 The project “The gathering and use of medical evidence in claims” has commenced and will aim to address this matter. The project is currently undertaking a review of the current practices in obtaining medical evidence for the claims process.
3.23 This is in conjunction with the work being undertaken by the manager of the Contracted Medical Advisers (CMAs) to further clarify the role and function of the CMAs, in order for DVA to best utilise their skills and expertise.
Are there appropriate quality assurance processes in R&C decision making?
DVA has an internal Quality Assurance function which conducts a statistically based review of all DVA activities. The error rate was above tolerable levels for 2016-17 in three of the six primary R&C claim categories.
3.24 There are three main mechanisms that provide insight into the quality of R&C decision making. These are:
- DVA’s Rehabilitation and Compensation Quality Assurance Program through the Service Delivery & Governance Section;
- formal reconsideration of decisions by DVA; and
- external review of decisions by the Veterans’ Review Board (VEA and MRCA) and the Administrative Appeals Tribunal (VEA, MRCA and DRCA).
3.25 In addition, DVA’s internal audit function has conducted reviews of the quality of decision making as part of the internal audit work program.
3.26 DVA’s Quality Assurance Program is a statistically based review of all DVA activities, including specific coverage of R&C. The reviews are conducted quarterly, results are provided to R&C management and corrective actions are taken where appropriate. The Quality Assurance Program covers:
- VEA;
- Initial Liability;
- Permanent Impairment;
- Incapacity;
- Rehabilitation; and
- Offsetting.
3.27 The Quality Assurance Program results for the financial year ending June 2017 are summarised in Table 3.3 below.
Table 3.3: Error rates from the Quality Assurance Program 2016-17
|
|
|
Financial year 2016-17 |
|
|||||
|
Claim type |
Cases checked |
Work elements |
Low Impact Errors |
Low Impact Error rate |
Low Impact Error tolerance |
High Impact Errors |
High Impact Error rate |
High Impact Error tolerance |
|
VEA |
363 |
835 |
80 |
9.6% |
10% |
40 |
4.8% |
5% |
|
MRCA Initial Liability |
108 |
400 |
14 |
3.5% |
10% |
20 |
5.0% |
5% |
|
DRCA Initial Liability |
96 |
175 |
13 |
7.4% |
10% |
25 |
14.3% |
5% |
|
MRCA Permanent Impairment |
84 |
368 |
30 |
8.2% |
10% |
14 |
3.8% |
5% |
|
DRCA Permanent Impairment |
72 |
132 |
8 |
6.1% |
10% |
12 |
9.1% |
5% |
|
MRCA/DRCA Incapacity |
312 |
603 |
95 |
15.8% |
10% |
99 |
16.4% |
5% |
Source: DVA Rehabilitation & Compensation Quality Assurance Reporting.
3.28 DVA identifies errors as Low Impact Errors (LIE) or High Impact Errors (HIE). HIE are defined by DVA as those that relate to the correctness of the decision or which have a financial impact more than $200. DVA has a stated tolerance for error of 5 per cent for HIE and 10 per cent for LIE for each different claim type. Details of errors are only reported to management where this tolerance is exceeded. For example, a 4.9 per cent error rate in the correctness of determinations would not be separately reported to management as part of the Quality Assurance Program reporting. The error rate was above tolerable levels, for 2016-17, in three of the six primary claim categories identified in the table above.
3.29 It should be noted that the calculation of error rates is based on a disaggregation of LIE and HIE. These errors are treated and analysed separately in management reporting. The error rates reported do not represent the total percentage of errors identified.
3.30 Error rate percentages are also measured against ‘work elements’ rather than cases. Each case is subdivided into a number of ‘work elements’ and as a result the error rates do not indicate the percentage of cases with identified errors. In 2016-17, for the claims analysed above, there were, on average, 2.4 ‘work elements’ examined for each case. The error rates for cases would be higher than the rates reported for ‘work elements’. The estimate of HIE against cases rather than ‘work elements’ is shown in Table 3.4 below.
Table 3.4: Analysis of error rates from the Quality Assurance Program 2016-17
|
|
Financial Year 2016-17 |
||
|
Claim type |
High Impact Errors |
High Impact Error rate |
Error rate for cases checked |
|
VEA |
40 |
4.8% |
11.0% |
|
MRCA Initial Liability |
20 |
5.0% |
18.5% |
|
DRCA Initial Liability |
25 |
14.3% |
26.0% |
|
MRCA Permanent Impairment |
14 |
3.8% |
16.7% |
|
DRCA Permanent Impairment |
12 |
9.1% |
16.7% |
|
MRCA/DRCA Incapacity |
99 |
16.4% |
31.7% |
Source: DVA Rehabilitation & Compensation Quality Assurance Reporting.
Veterans’ Review Board and Administrative Appeals Tribunal
3.31 External review of DVA decisions is undertaken by the Veterans’ Review Board (VRB) and the Administrative Appeals Tribunal (AAT). The VRB and AAT will often have access to information and statements by the claimant not made available to DVA.
3.32 In 2016-17, 46.7 per cent of all decisions referred to the VRB were set aside and 33.9 per cent of decisions referred to the AAT in 2016-17 were set aside. This is summarised in the tables below.
Table 3.5: Outcome of Veterans’ Review Board decisions 2011 to 2017
|
Outcome of review |
2016-17 |
2015-16 |
2014-15 |
2013-14 |
2012-13 |
2011-12 |
|
Total all matters |
2,356 |
2,331 |
2,449 |
2,476 |
2,674 |
2,941 |
|
Affirmed |
1,100 |
1,196 |
1,443 |
1,276 |
1,403 |
1,395 |
|
Affirmed (%) |
46.7% |
51.3% |
58.9% |
51.5% |
52.5% |
47.4% |
|
Set aside |
1,256 |
1,135 |
1,006 |
1,200 |
1,271 |
1,276 |
|
Set aside (%) |
53.3% |
48.7% |
41.1% |
48.5% |
47.5% |
43.4% |
Source: AAT Annual Reports.
Table 3.6: Outcome of Administrative Appeals Tribunal decisions 2011 to 2017
|
Outcome of review |
2016-17 |
2015-16 |
2014-15 |
2013-14 |
2012-13 |
2011-12 |
|
Total all matters |
59 |
78 |
113 |
95 |
90 |
117 |
|
Affirmed |
39 |
45 |
67 |
68 |
54 |
65 |
|
Affirmed (%) |
66.1% |
57.7% |
59.3% |
71.6% |
60.0% |
55.6% |
|
Varied or set aside |
20 |
33 |
46 |
27 |
36 |
52 |
|
Varied or set aside (%) |
33.9% |
42.3% |
40.7% |
28.4% |
40.0% |
44.4% |
Source: AAT Annual Reports.
3.33 It is important that DVA review the results of VRB and AAT reviews to ensure its systems maintain appropriate levels of quality.
3.34 In 2014 Internal Audit conducted a Review of Processing Consistency (SRCA-MRCA) – 2013-14 #08. This report concluded that ‘Incapacity testing by DS&R [the then Determination Support & Review Branch] continues to reveal a high error rate. Many of these errors reflect a failure to follow the approved national procedures and supplied checklists’. These findings from 2014 are consistent with the ANAO findings in this report.
Is the monitoring, reporting and analysis of Rehabilitation and Compensation operations supporting effective management?
An extensive suite of reports and analysis is prepared at various frequencies containing key metrics and analysis on R&C operations. This reporting has limited analysis about emerging risks or the reasons behind changes in performance. Management reporting does not identify progress on claims or the reasons for any delays, and is largely unutilised by team leaders.
3.35 Governance and oversight of R&C is the responsibility of a national business manager located in Melbourne. An extensive suite of reports and analysis is prepared on a monthly, weekly and daily basis containing metrics about R&C operations. The reports focus on the caseload, staffing, claims intake and TTTP broken down by locations and individuals. The standard reports also include exception reporting of all cases with a TTTP of 240 days or longer, 365 days or longer and separate reporting of the ‘top 20’ oldest claims. Along with TTTP reporting, the standard suite of reports provide details of quality assurance activities and results.
3.36 The nature of the reporting is focused on where and how problems may have already realised in R&C operations. Apart from reporting on the ‘extreme’ cases (greater than 240 days and 365 days) there is no analysis of any emerging problematic claims or the reasons behind changes in performance. Management reporting does not identify progress on claims or the reasons for any delays.
3.37 The governance and oversight reporting is separate from, and different to, the information used by team leaders to manage the delivery of services within the processing modules. Typically, team leaders use an ad hoc approach to managing their team’s efforts through consideration of individual case allocation, case conferencing and discussion of the circumstances surrounding individual cases. The team level management information is inconsistent and difficult to aggregate for higher level reporting, and to identify trends and systemic issues across R&C operations.
3.38 All reporting, both at the governance and team level, is focused on the processing modules. There is limited detail or aggregate reporting focused on the end-to-end R&C processes as a whole.
3.39 Reporting is based on data extracted from ISH and other systems, which do not provide visibility of potentially problematic claims and are separate from the team level reporting. DVA is currently implementing a new reporting system (RACER). DVA has indicated that much of its reporting will be changed and improved with the implementation of the RACER system later in 2018.
Recommendation no.6
3.40 The ANAO recommends that DVA develop and implement R&C reporting into its RACER system that:
- will allow the identification of claims that are potentially problematic at an individual claim level for operational management and at an aggregated level for oversight and governance; and
- provides transparent flow of consistent information at levels suitable for governance, module management and team and individual performance management.
Department of Veterans’ Affairs response: Agreed.
3.41 Reporting requirements are being scoped, with metrics related to processing milestones, timeframes, and quality as well as capturing data regarding the client experience, building on the client segmentation analysis undertaken by VCR. This is proposed as a future ICT development work for RACER.
How do DVA’s Rehabilitation and Compensation processes compare to similar entities?
The significant reorganisation of R&C operations following the creation of a national R&C business in 2015 has meant that internal benchmarking by location does not currently provide reliable comparisons. Comparisons between processing locations will become more reliable, as measures relative efficiency, when more comparable data becomes available.
Comparisons between DVA and Comcare show significant differences in approach to claims processing. However, there may be value to DVA in implementing comparisons going forward based on trends or detailed processes.
Comparison between processing locations
3.42 DVA prepares regular reports that include information about the TTTP within the processing modules to track performance across all of DVA’s R&C processes and locations. DVA has specialised processing centres and there is limited crossover between claim type and location. This is illustrated in Table 3.7 below.
Table 3.7: Processing of claim types by location
|
|
Processing location |
||||
|
Claim typea |
Melbourne |
Brisbane |
Perth |
Sydney |
Adelaide |
|
VEA |
✔ |
N/A |
N/A |
N/A |
N/A |
|
MRCA Initial Liability |
✔ |
N/A |
N/A |
✔ |
N/A |
|
DRCA Initial Liability |
✔ |
N/A |
N/A |
N/A |
N/A |
|
MRCA Permanent Impairment |
N/A |
✔ |
✔ |
N/A |
N/A |
|
DRCA Permanent Impairment |
✔ |
✔ |
✔ |
N/A |
N/A |
|
MRCA/DRCA Incapacity |
N/A |
✔ |
✔ |
N/A |
✔ |
Note a: The table only includes the claim types that were subject to analysis and testing as part of this audit. Not all claim types have been included.
Source: ANAO analysis of DVA processes.
3.43 The ANAO analysed processing performance for the claim type and locations for MRCA Initial Liability and Permanent Impairment to assess whether there were performance differences between locations.
3.44 Key metrics for MRCA Initial Liability claims processing for the period December 2016 to December 2017 for Melbourne and Sydney are set out below.
Table 3.8: MRCA Initial Liability key processing metrics by location
|
|
National |
Melbourne |
Sydney |
|||
|
National R&C Governance Reporting |
Dec-16 |
Dec-17 |
Dec-16 |
Dec-17 |
Dec-16 |
Dec-17 |
|
On Hand (at end) |
2,482 |
2,208 |
1,417 |
1,155 |
1,065 |
1,053 |
|
Mean TTTP of Claims Disposed (days) |
99 |
75 |
102 |
69 |
94 |
86 |
|
Mean Age of Claims On Hand (days) |
78 |
72 |
88 |
69 |
64 |
74 |
|
FTE (Cost Basis) |
22.9 |
39.2 |
9.0 |
19.2 |
13.9 |
20.0 |
|
Claims Disposed / FTE / week (Gross) |
6.9 |
4.1 |
10.2 |
5.2 |
4.8 |
3.0 |
|
Caseload per FTE |
109 |
56 |
157 |
60 |
77 |
53 |
Source: DVA Rehabilitation & Compensation National Reporting.
3.45 Table 3.8 indicates that in both Melbourne and Sydney the TTTP for claims is falling, as is the number of claims on hand. In both locations the mean age of claims on hand is also falling.
3.46 The assessment of relative performance between Melbourne and Sydney needs to take account of the fact that there was a significant reorganisation of resourcing and processing between 2016 and 2017. Staffing in Melbourne for MRCA Initial Liability increased from 9 Full Time Equivalent (FTE) to 19.2 FTE, and in Sydney staffing increased from 13.9 FTE to 20 FTE (44 per cent).
3.47 Key metrics for MRCA Permanent Impairment claims processing for the period December 2016 to December 2017 for Brisbane and Perth are set out in Table 3.9 below.
Table 3.9: MRCA Permanent Impairment key processing metrics by location
|
|
National |
Brisbane |
Perth |
|||
|
National R&C Governance Reporting |
Dec-16 |
Dec-17 |
Dec-16 |
Dec-17 |
Dec-16 |
Dec-17 |
|
On Hand (at end) |
2,587 |
1,543 |
2,144 |
787 |
443 |
756 |
|
Mean TTTP of Claims Disposed (days) |
161 |
71 |
182 |
68 |
129 |
73 |
|
Mean Age of Claims On Hand (days) |
137 |
71 |
142 |
72 |
116 |
71 |
|
FTE (Cost Basis) |
28 |
21.9 |
18.2 |
8.9 |
9.8 |
13 |
|
Claims Disposed / FTE / week (Gross) |
3.3 |
6.1 |
3.1 |
6.8 |
3.6 |
5.6 |
|
Caseload per FTE |
92 |
70 |
118 |
88 |
45 |
58 |
Source: DVA Rehabilitation & Compensation National Reporting.
3.48 The above table indicates that in both Brisbane and Perth the TTTP for claims is falling, as is the number of claims on hand. In both locations the mean age of claims on hand is also falling. The assessment of relative performance between Brisbane and Perth takes into account the fact that there was a significant reorganisation of resourcing and processing between 2016 and 2017. Staffing in Brisbane for MRCA Permanent Impairment decreased from 18.2 FTE to 8.9 FTE, which is a decrease of 57 per cent, and in Perth staffing increased from 9.8 FTE to 13 FTE (33 per cent).
3.49 The significant reorganisation of the R&C operations following the creation of a national R&C business in 2015 has meant that internal benchmarking by location does not provide reliable comparisons. However, there would be value for DVA in using location based comparative data in the future to develop metrics of relative efficiency.
Comparisons with Comcare
3.50 Claims processing under MRCA and DRCA have been compared by DVA to claims processing under the Safety, Rehabilitation and Compensation Act 1988 (SRCA) administered by Comcare.
3.51 The key performance indicators for Comcare include timeframes for the determination of claims. These are that 75 per cent of claims to be determined within:
- 20 days for injury; and
- 60 days for disease.
3.52 Whilst these timeframes are significantly shorter than target timeframes for MRCA and DRCA processing in DVA, there are differences between the schemes. These include:
- Comcare begins counting against its targets when a claim is received that is ‘ready for processing’, whilst DVA starts recording time from the receipt of the claim
- generally Comcare claims are submitted within 110 days of the incident or disease occurring, compared with the DRCA and MRCA average of 16 years;
- unlike Comcare, DVA is required to obtain and validate information from the Department of Defence and other third parties to support its investigation of claims.
3.53 The differences between claims processing in DVA and Comcare mean that the comparisons are unreliable in absolute terms. It would be valuable for DVA to implement more detailed or trend comparisons with Comcare going forward (for DRCA claims) which would provide DVA with insight into its relative performance.
Appendices
Appendix 1 Entity response

Appendix 2 Testing performed
The Australian National Audit Office (ANAO) performed testing over a limited sample of Rehabilitation and Compensation (R&C) claims. The sample was drawn from data relating to Veterans’ Entitlements Act 1986 (VEA), Military, Rehabilitation and Compensation Act 2004 (MRCA) and Safety, Rehabilitation and Compensation (Defence-related Claims) Act 1988 (DRCA) claims disposed between 1 October 2017 and 31 December 2017.
The data was provided by DVA and included data for all R&C claim types.
The data population is summarised below.
Table A.1: Data used to extract the sample
|
|
Total claims disposed between 1 October 2017 and 31 December 2017a |
||
|
Legislation |
Initial liability |
Permanent impairment |
Incapacity |
|
VEA |
1,165 |
N/A |
N/A |
|
MRCA |
2,430 |
1,421 |
444 |
|
DRCA |
1,931 |
1,270 |
94 |
|
Total |
5,526 |
2,691 |
538 |
Note a: Excludes cases with 0 days recorded.
Source: ANAO analysis of DVA claims disposed between 1 October 2017 and 31 December 2017.
The ANAO tested 53 claims as follows: 50 were with a high18 time taken to process (TTTP) and three selected randomly. The sample was selected from claims that were disposed in the period 1 October 2017 to 31 December 2017. The 53 claims sampled related to the following R&C claim types as outlined below. The sample did not include all VEA claim types or Incapacity and Rehabilitation claims.
Table A.2: Breakdown of sample for high time taken to process transactions
|
Claim type |
Number of claims |
|
VEA Disability Pension |
10 |
|
MRCA Initial Liability |
10 |
|
DRCA Initial Liability |
10 |
|
MRCA Permanent Impairment |
12 |
|
DRCA Permanent Impairment |
11 |
|
Total sampled |
53 |
Source: ANAO analysis of DVA claims disposed between 1 October 2017 and 31 December 2017.
The sample extraction was judgemental. The ANAO specifically targeted transactions with the highest TTTP within each of the claim categories. The sample was drawn in this way to facilitate the identification of characteristics that would lead to longer processing times for each type of claim, as shown in Figure A.1 below. In addition, during fieldwork the ANAO reviewed claims with DVA staff to understand the processes and factors that influenced overall processing time for claims. Discussions included claims with low TTTP to understand the characteristics that would lead to shorter processing times for claims.
Figure A.1: Example sample selection for DRCA Permanent Impairment
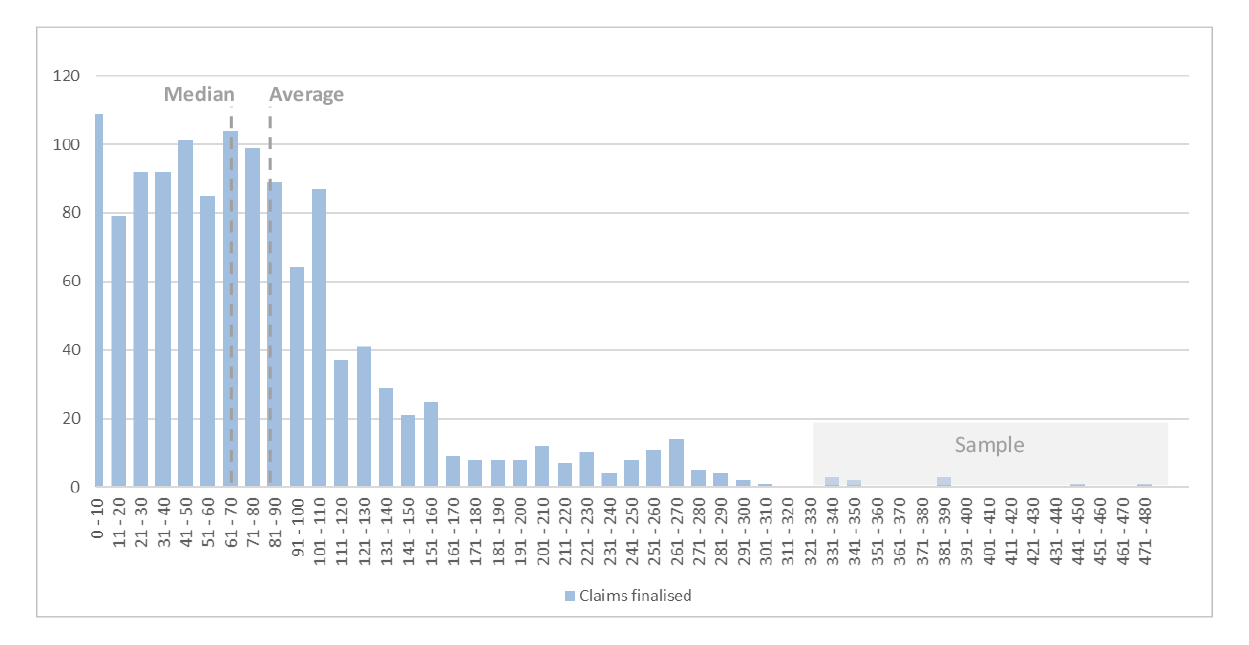
Source: ANAO analysis of DVA claims disposed between 1 October 2017 and 31 December 2017.
For each of the high TTTP claims tested, the ANAO reviewed documentation included on the official file to determine processing steps and actions taken in relation to the individual claim. For each claim the ANAO recorded information (where it was available) related to the circumstances and nature of the claim, staff members involved in processing the claim and the dates when:
- the claim was received;
- the claim was registered;
- there was communication and correspondence with the client;
- information requests were sent;
- information requests were received; and
- the determination was made.
The ANAO prepared a claim chronology or ‘clock’ that categorised the time spent processing the claim. The analysis identified active time, waiting time and inactive time between receipt and determination (or other disposition) of the claim.
It should be noted that the sample testing should not be extrapolated to the population of R&C claims generally, and it is unlikely to be representative of that population.
Appendix 3 DVA national reporting of median and trend information for disposed claims February 2017 to February 2018
The figures below provide further examples of DVA’s performance reporting for February 2018.
Figure A.2: National IS Claims Median Disposed & Trend (Chart 1a)
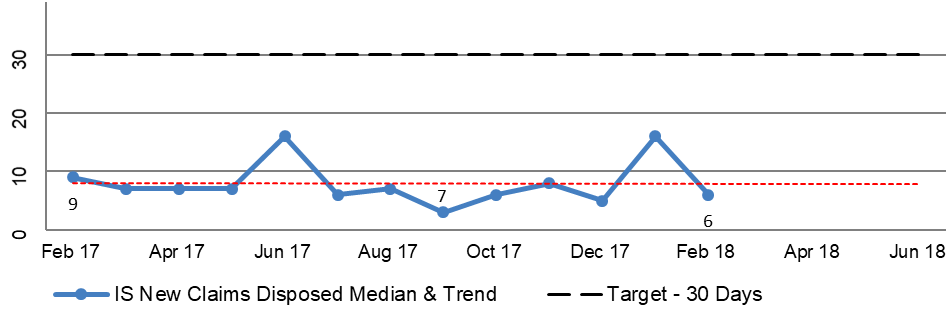
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.3: National IS PIR’s Median Disposed & Trend (Chart 2a)
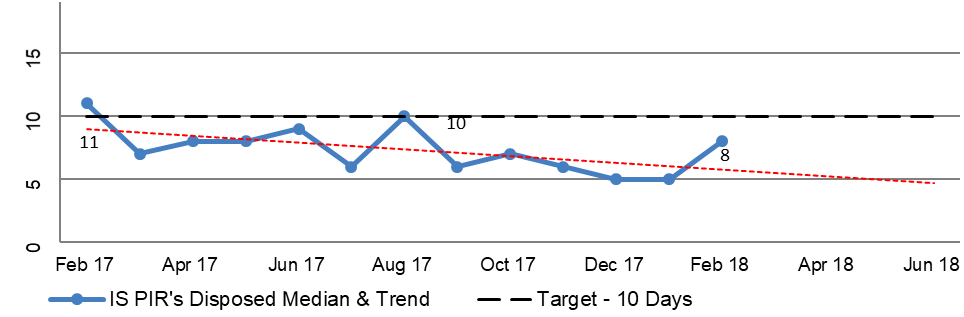
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.4: National VEA DP Median Disposed & Trend (Chart 3a)
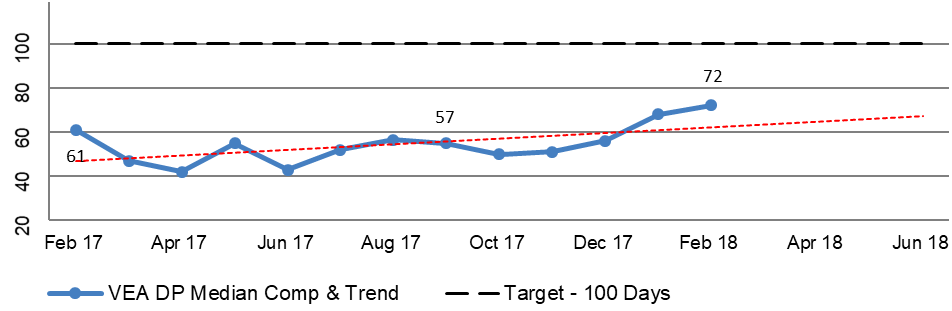
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.5: National VEA War Widows Disposed Median & Trend (Chart 4a)
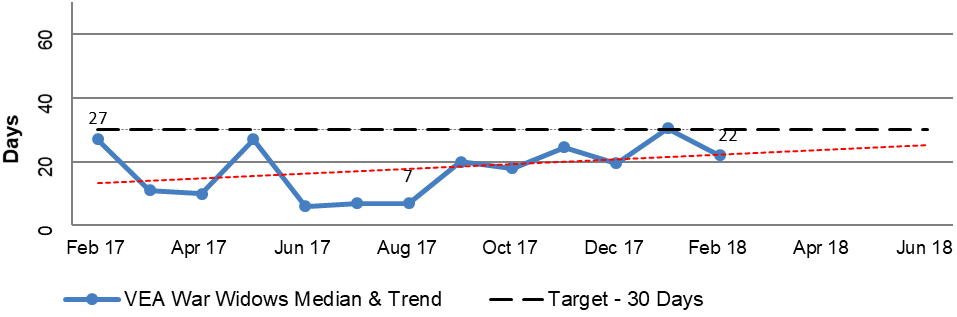
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.6: National SRCA IL Median & Trend (Chart 6a)
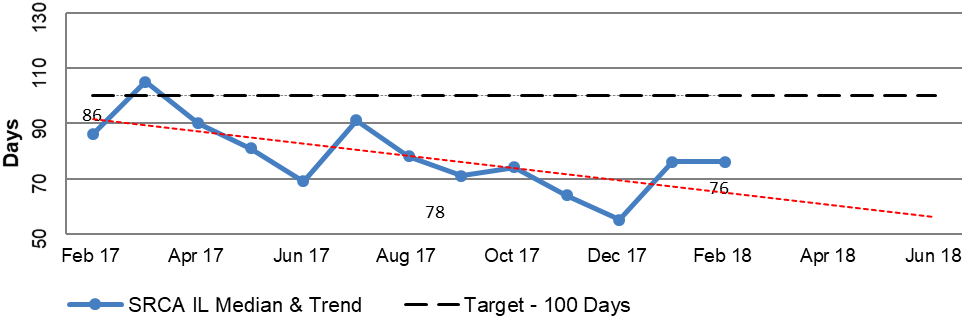
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.7: National SRCA PI Median & Trend (Chart 8a)
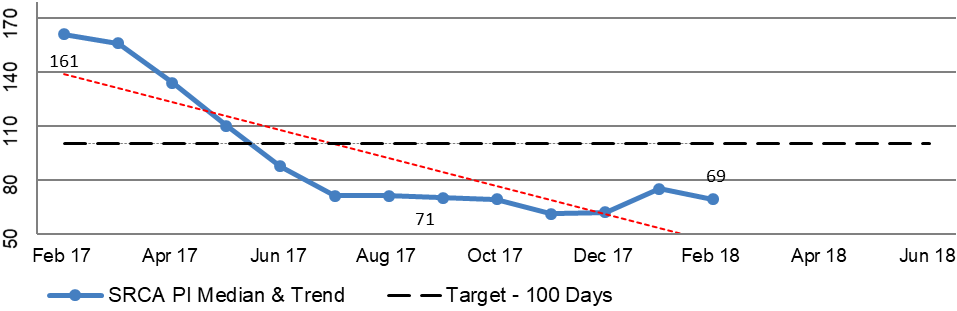
Source: DVA Rehabilitation & Compensation National Reporting.
Figure A.8: National SRCA Incap Median & Trend (Chart 10a)
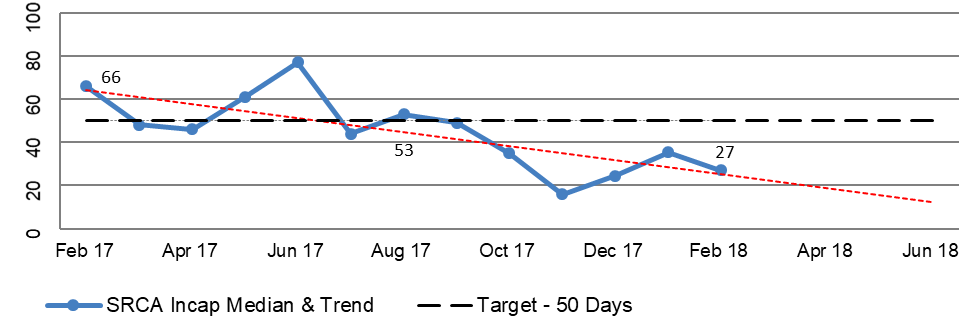
Source: DVA Rehabilitation & Compensation National Reporting.
Appendix 4 Disposals between 1 October 2017 and 31 December 2017 above 240 days and 365 days
The following table shows the numbers disposed with a time taken to process of greater than 240 days and 365 days respectively.
Table A.3: Disposals of claims between 1 October 2017 and 31 December 2017 with time taken to process greater than 240 days
|
|
Number of claims |
|
|
Claim module |
Over 240 days for segment |
Over 365 days for segment |
|
MRCA Initial Liability |
20 |
1 |
|
DRCA Initial Liability |
73 |
2 |
|
MRCA Permanent Impairment |
10 |
2 |
|
DRCA Permanent Impairment |
55 |
5 |
|
Total |
158 |
10 |
Source: ANAO analysis of DVA claims disposed between 1 October 2017 and 31 December 2017.
Footnotes
1 This is typically expressed as differences in the burden of proof of claims made; DRCA is ‘beyond reasonable doubt’ for all service types whereas for VEA and MRCA it is ‘reasonable satisfaction’ for Warlike and Non-Warlike service.
2 Department of Veterans’ Affairs, Budget 2017-18 Veteran Centric Reform, page 1. Available from <https://www.dva.gov.au/sites/default/files/files/about%20dva/budgets/2017-18/veterancentricreform.pdf>.
3 The purpose [of a Gateway Review] is to provide the Senior Responsible Officer with independent assurance and advice to improve the delivery and implementation of … policies, programmes, projects, and services, as well as providing an early identification of areas requiring corrective action. Available from <https://www.finance.gov.au/assurance-reviews/review-process/>.
4 Resource Management Guide 106 defines a ‘Green/Amber’ rating as ‘Successful delivery of the program/project to time, cost, quality standards and benefits realisation appears probable however constant attention will be needed to ensure risks do not become major issues threatening delivery’. Available from <https://www.finance.gov.au/assurance-reviews/guidance-on-assurance-reviews/>.
5 Statements of Principles determined by the Repatriation Medical Authority are legislative instruments and have the same legal effect as any legislation passed by Parliament. SOPs exclusively state what factors must exist to establish a causal connection between particular diseases, injuries or death and service. Available from <http://www.rma.gov.au/sops/>. The SOPs apply to decisions about liability for injuries, diseases and deaths made under both the Veterans’ Entitlements Act 1986 and the Military Rehabilitation and Compensation Act 2004.
6 The Department has implemented straight-through processing arrangements for certain liability claims. Under this arrangement, training and service data provided by Defence are used to satisfy specified Statements of Principles factors for certain medical conditions. Where straight-through processing is applicable, claimants will no longer be required to fill out questionnaires detailing their specific service activities, potentially reducing the time taken to assess liability.
7 Needs Assessment is the process to determine how to meet an accepted need of the veteran. Available from <https://www.dva.gov.au/factsheet-mrc34-needs-assessment>.
8 In this report the ANAO has used the following terminology; medical specialists refers to treating medical specialists who have a direct relationship with the client and independent medical specialists engaged directly by DVA. Contracted Medical Advisors are medical personnel located on site in DVA offices and advise on reports provided by medical specialists.
9 DVA, Clik, Determining a Claim, Reasonable hypothesis (RH) cases. Available from <http://clik.dva.gov.au/military-compensation-mrca-manuals-and-resources-library/policy-manual/ch-3-liability/35-determining-claim/353-reasonable-hypothesis-rh-cases>.
10 DVA, Review of Military Compensation Arrangements, February 2011. Available from <https://www.dva.gov.au/consultation-and-grants/reviews/review-military-compensation-arrangements>.
11 It should be noted that the DVA is currently piloting a process where Needs Assessment is carried out before the Initial Liability assessment.
12 APH, The Constant Battle: Suicide by Veterans, August 2017. Available from <https://www.aph.gov.au/ Parliamentary_Business/Committees/Senate/Foreign_Affairs_Defence_and_Trade/VeteranSuicide/Report>.
13 Until recently DVA’s TTTP targets were all expressed as ‘means’ or averages. For the 2017-18 financial year onward, DVA will report primarily on the ‘median’ TTTP target times. At the process level, mean or average targets continue to be used extensively.
14 Median is the value lying at the midpoint of a frequency distribution. In DVA’s case, it expresses the time taken to process 50% of the claims.
15 Internal governance reports contain a wide range of performance information, including:
- period and year-to-date claims on hand; period and year-to-date median TTTP;
- period and year-to-date average TTTP;
- period claims intake;
- period claims acceptance;
- period claims rejections;
- claims on hand over 240 days;
- claims on hand over 365 days; and
- period quality assurance error rates.
16 ‘A condition which is the consequence of a previous disease or injury.’ Available from <https://en.oxforddictionaries.com/definition/us/sequela>.
17 It is important to note that the ‘older than 240 days’ refers to process segments or modules for each of these claims, not end-to-end processing of the claim. This is illustrated in Appendix 4.
18 The claims selected were the 10 with the longest TTTP in each of the claim types sampled. The claims sampled had a TTTP between 243 and 755 days when disposed.